
Expired activity
Please go to the PowerPak
homepage and select a course.
Chronic Idiopathic Constipation: Incorporating Newer Agents Into Evidence-Based Care
INTRODUCTION
Functional or chronic idiopathic constipation (CIC) is one of the most common chronic functional gastrointestinal (GI) disorders worldwide. The incidence of CIC is difficult to determine. A population-based study reported the incidence of CIC between 1998 and 2003 to be 17.4%.1 Prevalence of CIC has been estimated between 1.9% to 40.1%, with a mean prevalence of approximately 14%.2 Female sex, older age, lower socio-economic status, reduced caloric intake, sedentary lifestyle, and reduced dietary fiber intake elevate risk.3
CIC imposes a significant economic burden to the health care system. In the United States, reported direct costs per patient have varied widely but have been estimated to range from $1912 to $7522 annually.3
According to the Rome IV diagnostic criteria for functional GI disorders, a diagnosis of CIC or functional constipation must include 2 or more of the following during the last 3 months with symptom onset of at least 6 months4:
1. Straining during more than 25% of bowel movements (BMs)
2. Lumpy or hard stools in 25% of BMs
3. Sensation of incomplete evacuation in more than 25% of all BMs
4. Sensation of anorectal blockage or obstruction in more than 25% of BMs
5. Manual maneuvers required in more than 25% of BMs
6. Fewer than 3 BMs per week
In addition to having at least 2 of the above criteria, the following must also apply4:
1. Loose stools are rarely present without the use of laxatives
2. Insufficient criteria for irritable bowel syndrome (IBS)
Since CIC's symptoms are often confused and may overlap to some extent with IBS, the Rome IV criteria for diagnosis also clarify that patients with CIC may have bloating and mild abdominal pain, but that these symptoms should not predominate as they do in IBS patients.4 Although the Rome IV criteria consider CIC and IBS separate entities, abundant accumulating evidence suggests that these are manifestations along a disease continuum. Differential diagnosis may not only be difficult, but patients may actually move between diagnoses over time, switching from IBS to CIC or the reverse.4
Case Study
Susan is a 42-year-old woman who presents to clinic with a chief complaint of constipation. Over the past 8 to 9 months, she has noticed increased difficulty in having complete bowel movements. She states that she occasionally feels bloated and has a general feeling of discomfort. When she does have a bowel movement, she states that she usually has to strain and generally does not feel like the movement was complete. Susan states she has 2 to 3 bowel movements a week. When she has a successful movement, the stool is typically hard. Based upon the information provided, does Susan meet the Rome IV criteria for CIC diagnosis?
PATHOPHYSIOLOGY
After ruling out secondary causes of constipation such as medications (e.g., opiates, anticholinergics), endocrine disorders (e.g., hypothyroidism, diabetes mellitus), autonomic neuropathies, eating disorders, and mechanical obstructions, clinicians diagnose CIC based on symptoms. They differentiate it from IBS with constipation (IBS-C) by the absence of persistent pain and abdominal distention.
The etiology of CIC and IBS are complex and may involve a number of psychosocial and physical changes. Limited studies from pediatric populations suggested that lifestyle factors in childhood including low fiber intake, low fluid intake, and ignoring the call to defecate may contribute to chronic constipation.4 Slow transit due to decreased autonomic nervous system effects, decreased colonic smooth muscle activity, or decreased colonic “pacemaker” cell activity may cause CIC.4,5
In dyssynergic defecation disorders, the pelvic floor muscles, abdominal muscles and recto-anal muscles coordinate poorly because of decreased colonic propulsive force or increased anal sphincter resistance.5
PATIENT EVALUATION
Patients with chronic constipation complain most frequently of the following symptoms: straining, hard stools, bloating, abdominal discomfort, infrequent bowel movements, and the feeling of incomplete bowel evacuation after a bowel movement.6 In addition to symptoms reported by the patient, a thorough medical history may help discern other potential causes such as endocrine disorders, obstructions, and medication use.
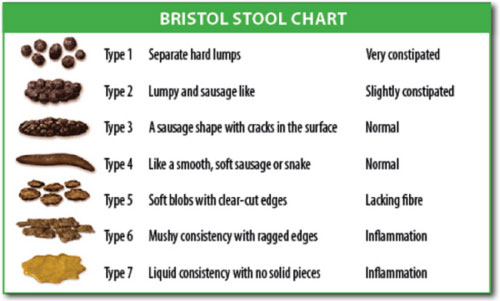
The patient history should include information on bowel movement frequency; stool consistency assessed using the Bristol Stool Form Scale (BSFS; see Figure 1); symptom duration; and associated symptoms such as pain and bloating and stool size. The BSFS is a useful way to assess stool form as it aids differential diagnosis between slow transit constipation and dyssynergic defecation; bowel movements with more loose stool (e.g., type 5 or 6) and straining may indicate obstruction, whereas type 1 stool may indicate slower transit.4,5
| Figure 1. The Bristol Stool Form Scale7 |
 |
| This file is licensed under the Creative Commons Attribution-Share Alike 3.0 Unported license |
Alarm features may include a family history of colon cancer, rectal bleeding, or dramatic weight loss. A physical examination may include assessment of the spinal cord and central nervous system. The clinician should assess the patient's abdomen for hard stool and masses. Digital rectal examinations may indicate fecal impaction, strictures, or rectal masses. In addition, laboratory values including thyroid panels, blood glucose, calcium, and complete blood counts can identify secondary causes of constipation. Diagnostic measures that document colon transit time and rectal expulsion pressures are described elsewhere in recent reviews.4,5
TREATMENT OF CIC
The treatment goal in CIC is to relieve patients’ altered bowel habits by increasing the frequency of spontaneous and complete BMs, providing a sense of complete evacuation.8 In this and the following section, currently available and investigational agents for CIC are reviewed (Tables 1 and 2). Nonprescription agents are important components of an effective regimen in CIC. The U.S. Food and Drug Administration (FDA) has approved three prescription agents for treatment of CIC: lubiprostone, linaclotide, and plecanatide. A number of agents from different drug classes are in clinical trials. These include serotonin receptor agonists, an inhibitor of the Na+/H+ exchanger, an inhibitor of bile acid transport, and a synthetic ghrelin analog.
| Table 1. Over-the-Counter Medications for CIC11 |
| Drug Category |
Generic Name |
Dosing |
Quality of Evidence* |
Adverse Effects |
| Bulking laxatives/soluble fiber |
Psyllium |
2.4 g 1–3 times/day |
Strong/low |
Diarrhea, abdominal pain, cramping, esophageal obstruction possible if administered with insufficient liquid |
| Osmotic laxatives |
Polyethylene glycol |
17 g once/day |
Strong/high |
Flatulence, nausea, diarrhea |
| Stimulant laxatives |
Bisacodyl |
5–15 mg once/day |
Strong/moderate |
Abdominal pain, cramping, nausea, vomiting, electrolyte imbalances |
| * American College of Gastroenterology recommendations are based on the GRADE (Grading of Recommendations Assessment, Development and Evaluation) system. The recommendation is rated as strong or weak according to the quality of evidence, applicability to all patient groups, balance of risks and benefits, patient preferences, and cost; a recommendation rated as strong can apply to most patients in most circumstances. Quality of evidence is rated as high, moderate, low, or very low depending on the extent to which further evidence would change the estimate of treatment effect. |
| Table 2. Emerging Agents for Treatment of CIC and/or IBS-C |
| Drug Class |
Agent |
Clinical Trial Phase* |
Key Efficacy Findings |
Key Safety Findings |
Comments |
| 5-HT4 receptor agonist |
Prucalopride |
Phase 3 |
↑CSBMs; ↑QOL; ↑satisfaction with bowel function |
Headache, nausea, abdominal pain, cramps, diarrhea; no hemodynamic or electrocardiographic changes |
Three phase 3 trials completed; approved by EMA for women only |
| Naronapride |
Phase 3 |
↑SBMs; ↓time to first BM |
Headache, abdominal pain (only higher doses) |
Phase 2 trials completed, entering Phase 3 |
| Velusetrag |
Phase 3 |
↑SBMs; ↑CSBMs |
Diarrhea, headache, nausea, and vomiting |
Phase 2 trials completed for gastroparesis and CIC |
| NHE3 sodium transporter inhibitor |
Tenapanor |
Phase 3 (IBS-C) |
↑SBMs; ↑CSBMs; reduced pain, discomfort, bloating, cramping, fullness |
Diarrhea, headache, nausea, abdominal pain, flatulence |
New drug application submission expected in 2018 |
| Bile acid transport inhibitor |
Elobixibat |
Phase 3 |
↑SBMs; ↑CSBMs; ↑BSFS score |
Abdominal pain, diarrhea |
May improve serum lipid profiles |
| Ghrelin GHS1a receptor agonist |
Relamorelin |
Phase 3
(gastroparesis)
Phase 2 (CIC) |
↑Gastric emptying rate; ↑SBMs; ↓Colonic transit time; ↓time to first BM |
↑Appetite, fatigue, headache |
May increase hyperglycemia, unknown cancer risk |
| *Clinical Trial Phase for CIC indication unless otherwise noted. Abbreviations: BSFS, Bristol Stool Form Scale; CIC, chronic idiopathic constipation; CSBM, complete spontaneous bowel movement; EMA, European Medicine Agency, GHS, growth hormone secretagogue; IBS-C, irritable bowel syndrome with constipation; NHE, sodium proton exchanger; QOL, quality of life; 5-HT, serotonin; SBM, spontaneous bowel movement. |
Self-care Interventions
Treatment options for CIC include lifestyle modifications such as increased physical activity and increased dietary fiber.9,10 Dietary modifications beyond increasing fiber have not been well studied for this condition. The American College of Gastroenterology recently published a monograph on the management of CIC; other than dietary fiber, no dietary modifications were reviewed.11
At least one trial has evaluated exercise's impact on chronic constipation. This small study (n =43) evaluated the effect of a 12-week exercise program on transit time and defecation in adult patients. The exercise program consisted of 30 minutes of walking and an at-home regimen that took approximately 10 minutes a day. At the end of the 12-week period, both transit time and defecation patterns significantly improved.10 Clinicians should encourage patients who have no contraindications to exercise to maintain an active, healthy lifestyle.
For decades, clinicians have recommended over-the-counter (OTC) products to treat CIC, including bulking agents (e.g., psyllium, methylcellulose, calcium polycarbophil), osmotic laxatives (e.g., magnesium hydroxide, polyethylene glycol), stool softeners (e.g., docusate sodium) and stimulant laxatives (e.g., senna, bisacodyl).11 Soluble fiber (e.g., psyllium, inulin) may be preferred over insoluble fiber (e.g. bran) for CIC since insoluble fiber may produce more cramping, bloating, and flatulence.11
A recent systematic review with meta-analysis of the effects of fiber supplementation found that fiber significantly increased stool frequency and softened stool consistency compared with placebo, although flatulence was significantly higher in patients treated with fiber versus placebo.12 A recent review that analyzed 19 clinical trials and 4 meta-analyses determined that both stimulant and nonstimulant laxatives relieve constipation better than placebo according to both subjective and objective measures.13 Adults and children tolerated laxatives well. Of the osmotic laxatives, polyethylene glycol (PEG) was most effective compared with other osmotic agents. Patients found PEG without electrolytes more palatable than PEG with electrolytes and preferred it.13 Stimulant laxatives produced more diarrhea and abdominal distention than did nonstimulant laxatives and may therefore be less preferred for longer treatment of chronic constipation.13
Case Study
Because Susan had experienced symptoms for longer than 6 months and met at least 2 of the Rome IV criteria, she was diagnosed with CIC. Her physician referred her to the pharmacy for an OTC product. She would like your help selecting a product. She recalls the physician telling her the constipation therapies available OTC were all fine, but something may have been better than the others. She has a psyllium-based fiber supplement, docusate sodium, and PEG in her shopping basket. What information can you provide her regarding these products?
Investigational Agents
Serotonergic agents. The neurotransmitter serotonin (5-HT) is found in the central nervous system and the enteric nervous system. It regulates a number of responses within the GI tract. A total of 14 different 5-HT receptor subtypes have been identified. The 5-HT4 receptor subtype is important in regulation of GI motility and is expressed on enterochromaffin cells, smooth muscle cells, and afferent nerve fibers that help to initiate the peristaltic reflex.14 Activation of the 5-HT4 receptor enhances acetylcholine release from autonomic and enteric nerve terminals increasing motility and secretions within the GI tract.14
FDA approved tegaserod, a 5-HT4 agonist, in 2002 for short-term treatment of IBS-C in women. In 2004, FDA approved an additional indication for CIC in adults younger than 65 years. Because of cardiovascular toxicity, the manufacturer removed tegaserod from the U.S. market in 2007.14 It is currently available only as an emergency treatment for IBS-C or CIC in women younger than 55 and requires prior authorization by FDA.
Prucalopride is a 5-HT4 receptor agonist that has received approval for IBS-C, CIC, and opiate agonist-induced constipation (OIC) by the European Medicines Agency (EMA). It is available in Europe, Canada, Mexico, and other countries.5 Prucalopride is very selective for 5-HT4 receptors; limited activity at the HERG potassium channel, 5-HT1, and 5-HT2 receptors make this drug less likely to cause cardiotoxicity than tegaserod.14,15 It has less potential for drug-drug interactions because it is not metabolized by the cytochrome P450 pathway.14 In a systematic review with meta-analysis of 13 clinical trials, 11 of which included prucalopride dosed in more than 3,280 patients, prucalopride significantly increased the number of spontaneous bowel movements (SBM) and improved constipation quality of life indicators with no reported cardiovascular effects.16 In the United States, prucalopride has been tested in multiple phase 3 trials. At doses of 2 and 4 mg daily, prucalopride significantly increased the number of bowel movements/week compared with placebo. Pain, bloating, and need for laxatives were all significantly reduced.17 Prucalopride’s most common adverse effects included headache, abdominal pain, nausea, diarrhea, and flatulence. The diarrhea was reported to be transient and averaged 1.7 days in the 2 mg group and 3 days in the 4 mg group.17
Naronapride is a selective 5-HT4 agonist that has completed phase 2 studies. Naronapride is also a selective 5-HT4 agonist with little activity at other receptors and little reported cardiovascular toxicity.18 In a phase 2 study, naronapride at all doses (20, 40, 80, and 120 mg twice daily) resulted in a greater number of SBMs in week 1 compared with placebo. Median time to first SBM was reduced in all doses and significantly reduced at 40 and 80 mg doses. Patients treated with 120 mg twice daily reported abdominal pain and headache adverse effects that were significantly greater than placebo; all other doses reported adverse effects of nausea, diarrhea, abdominal pain, and headache that were similar to placebo.18
Velusetrag, another 5-HT4 selective agonist, has a binding and cardiovascular risk profile similar to naronapride and prucalopride.15 It has completed phase 2 trials for diabetic gastroparesis and CIC.19 Significant increases in SBMs per week were reported for all 3 doses (15, 30 and 50 mg). Statistically significant increases in the weekly frequency of complete spontaneous bowel movements (CSBMs) were also reported. Most common adverse effects were diarrhea, headache, nausea, and vomiting, generally limited to the initial days of dosing and were dose-dependent.20
Na+/H+ Exchange Inhibitors. Tenapanor (AZD1722/RDX5791) selectively inhibits Na+/H+ exchanger-3 (NHE3) that acts exclusively in the gut and prevents sodium reabsorption from the GI tract. It draws water into the GI tract, enhancing intestinal fluid volume and increasing the frequency of BMs and stool softness. Systemic exposure is limited.21 Tenapanor is currently in multiple phase 3 trials in the United States for IBS-C.20 Results of a phase 2 randomized, placebo-controlled efficacy and safety trial showed that tenapanor (5, 20, or 50 mg twice daily) increased stool frequency and increased CSBMs in a dose-dependent manner. It also reduced abdominal symptoms including pain, discomfort, bloating, cramping, and fullness.22 Tenapanor-treated patients reported more diarrhea, nausea, headache, and abdominal pain than those in placebo groups.22
Ileal bile acid transporter (IBAT) inhibitor. Elobixibat (A3309) is an IBAT inhibitor that prevents bile acid reabsorption by the GI tract through enterohepatic circulation. Thus, bile acids are trapped in the GI tract and draw water into the lumen by osmosis. In a phase 2b study in Japanese patients with chronic constipation, SBM frequency at week 1 were significantly increased in a 10 or 15 mg once-daily group compared with placebo. There was a dose-dependent increase in CSBMs and dose-dependent increase in BSFS stool type. Elobixibat-treated patients experienced more abdominal pain and diarrhea than placebo-treated patients.
Since bile acids are composed of cholesterol, the abundant hepatic synthesis of bile acids promotes up-regulation of low density lipoprotein (LDL) receptors in the liver, resulting in reduced serum LDL cholesterol levels. In a phase 2b study, serum LDL cholesterol concentrations were significantly reduced at all doses of elobixibat.23
Ghrelin analogs. Ghrelin is a 28-amino acid peptide first isolated from rat stomach. It is widely distributed throughout the GI tract. Theories suggest that it plays a role in hunger sensations by interacting with receptors in the hypothalamus.24 Ghrelin interacts with specific receptors known as growth hormone secretagogue 1a (GHS-1a) receptors expressed in hypothalamus and throughout the GI tract.
Ghrelin promotes gastric motility in rodents, dogs and humans. However, ghrelin’s very short half-life and instability in plasma limit its utility as a medication. Companies have been developing small molecule ghrelin agonists for years to test for GI motility disorders.24 Relamorelin, a pentapeptide ghrelin analog, possesses better plasma stability and half-life than ghrelin.24 It is more potent at the GHS-1a receptor than ghrelin itself. In human studies, relamorelin had a half-life of approximately 4.5 hours after subcutaneous dosing. Relamorelin does not interact appreciably with cytochrome P450 enzymes, minimizing its drug interaction potential.19
Relamorelin is currently in phase 3 trials for diabetic gastroparesis and has completed phase 2 trials for gastoparesis and for chronic constipation.19 In a phase 2 trial in female patients, relamorelin accelerated gastric-emptying half-time; decreased small bowel and colonic transit; increased the number of SBMs; and decreased time to first BM compared with placebo. However, the drug did not affect stool form. Adverse events of relamorelin included increased appetite, fatigue, and headache.25 Relamorelin's manufacturer is targeting diabetic gastroparesis as its primary indication, but several potential adverse effects are troubling. Increased appetite could exacerbate obesity and insulin resistance in patients with diabetes. Hyperglycemia, possibly resulting from increased gastric emptying rate and/or the drug's effects on growth hormone secretion, are also a concern.26 Since ghrelin may induce cell proliferation and angiogenesis, its potential influence on cancer cell proliferation is uncertain.
By stimulating appetite, ghrelin agonists may be useful in patients with cancer-induced cachexia, but the long-term safety of ghrelin agonists needs to be established to rule out any link to cancer progression.24 Future clinical trials will help to discern whether these adverse effects are clinically relevant.
CURRENT APPROACHES TO CIC
The goal of CIC treatment is to increase the frequency of CSBMs and SBMs. Therapy involves use of a number of different agents and selection is based upon 2 patient characteristic: transit time and pelvic floor dysfunction. Up to 60% of patients will have normal transit times, and need only symptomatic treatment.27 One approach to symptomatic care may be to first increase fiber intake. If there is no relief, a trial of an osmotic laxative may be warranted. Stimulant laxatives may be initiated if the osmotic laxative is unsuccessful. Secretagogue therapy is initiated if other modalities fail. Most patients will require a treatment regimen that contains both OTC and prescription agents (Table 3).28
| Table 3. Key Characteristics of Lubiprostone, Linaclotide, and Plecanatide34,37,39,42,43 |
| Agent |
Dosing |
Administration |
Efficacy |
Safety |
| Lubiprostone |
24 mcg |
Twice daily with food and water |
Improves frequency, consistency, and reduces straining |
Nausea, diarrhea, headache |
| Linaclotide |
145 mcg |
Once daily on an empty stomach 30 minutes before first meal of the day |
Increases CSBM; no additional benefit at higher dosing |
Diarrhea |
| Plecanatide |
3 mg |
Once daily without regard to food |
Increases CSBM; improves frequency and consistency |
Diarrhea |
| Abbreviation: CSBM, complete spontaneous bowel movement |
Intestinal Secretagogues
FDA approved lubiprostone in 2006 for the treatment of CIC, OIC, and IBS-C. This prostaglandin (PG) E-series analog acts locally and is almost completely metabolized in the intestinal lumen after oral administration. Lubiprostone has very poor systemic availability; plasma levels are undetectable after oral administration. It is rapidly metabolized to an active metabolite with a plasma half-life of about 1 hour. Lubiprostone is thought to bind and directly activate the chloride (Cl–) channel type 2 (ClC-2), resulting in increased chloride secretion. These increasing chloride secretions lead to passive sodium and water secretion and secretion of isotonic fluid into the intestinal lumen, which softens stool. In addition, enhanced GI motility mediated by lubiprostone may be attributed to either increased fluid content of the GI lumen or to a direct effect on smooth muscle contraction via activation of a prostaglandin E1 (EP1) prostanoid receptor.29
A recent meta-analysis evaluated 9 randomized, controlled trials and found that lubiprostone significantly improved symptoms and stool consistency as early as 1 week after beginning treatment (P ≤ 0.03). SBM frequency was significantly higher compared to placebo at 1 week and 1 month, but failed to maintain significance after 3 months of treatment (95% confidence interval, -0.127 – 0.4; P = 0.34). Symptom improvements related to bloating, straining, stool consistency, and severity of constipation were maintained after 1 month (P ≤ 0.004). Unfortunately, many gains in symptom improvement were lost after 3 months. Constipation severity and abdominal bloating were the only symptoms to maintain a significant difference compared to placebo at the 3 month time point (P = 0.05 and 0.03, respectively). Lubiprostone has also been shown to increase the number of SBMs significantly in patients with diabetes. Patients receiving lubiprostone had almost 2 more bowel movements a week compared with those on placebo (P = 0.02).30 Gastrointestinal effects (nausea, vomiting, diarrhea) are the most commonly reported adverse effects.31
Mild-to-moderate nausea appears to occur in approximately 30% of patients treated with lubiprostone. Most nausea is a single event that occurs within the first 5 days of therapy. Women and patients younger than 65 seem to experience more nausea than others. Clinicians should counsel patients to take lubiprostone with food and water to reduce the incidence of nausea.32 Clinicians should also educate patients that dyspnea is a rare adverse effect. It has been reported to occur within an hour of the first dose, but generally resolves within 3 hours. It may occur with subsequent dosing. Patients should speak with their healthcare provider if this occurs.33
Case Study
Susan has been using a psyllium-based fiber supplement and occasional bisacodyl rescues for her CIC. Since her symptoms have not improved greatly, she and her physician decide to begin a prescription agent. Her physician prescribes lubiprostone. Two days later, Susan calls you complaining of nausea. What counseling should you provide her to address this adverse effect?
FDA approved linaclotide (Linzess) in 2012 for CIC and IBS-C in both men and women. Linaclotide, a 14 amino-acid peptide, has minimal systemic exposure after oral administration. It is structurally very similar to a heat-stable enterotoxin produced by Escherichia coli. Its activity is pH-independent; it is stable in the acidic environment of the stomach and is rapidly converted in the small intestine to an active 13-amino acid metabolite with a half-life of 10 minutes. Linaclotide is degraded within the intestine to inactive amino acids; only 3% to 5% of an oral dose is excreted in feces as active peptide.34
Linaclotide mimics the effects of endogenous pro-secretory peptides found in the GI tract that serve to increase GI secretions after a meal. The endogenous peptides uroguanylin and guanylin bind to membrane-bound guanylate cyclase C (GC-C) receptors that function to convert guanosine triphosphate (GTP) to cyclic guanosine monophosphate (cGMP). cGMP is an intracellular second messenger that activates a protein kinase G type II (PKG II), which can subsequently phosphorylate numerous cellular targets, including the cystic fibrosis transmembrane conductance regulator (CFTR), which is a chloride channel similar to CIC-2 mentioned above. PKG II-mediated phosphorylation activates CFTR, leading to increased chloride secretion into the intestinal lumen and increased intestinal fluid entry into the GI tract.34
Evidence suggests that linaclotide stimulates cGMP transport by the multidrug resistance proteins type 4 and 5 (MRP4/5) out of epithelial cells into the submucosal space, allowing cGMP to decrease activity of afferent pain fibers.26 Compared with placebo, linaclotide significantly increases the percentage of patients who experience 3 or more CSBMs a week (P = 0.01). The 145 mcg and 290 mcg doses are associated with similar symptom improvement. Bloating, stool consistency, and straining also are significantly better with linaclotide than placebo. Patients with moderate-to-severe abdominal pain may experience greater pain reductions than patients with mild pain, even at the lower dose.34 Linaclotide use also decreases the percentage of patients who require rescue medication by approximately one half. Mild-to-moderate diarrhea is the most commonly reported adverse effect; it occurs more frequently in patients using the higher dosage.35,36
FDA approved plecanatide in 2016 for CIC. Structurally, it is very similar to uroguanylin, different by only one amino acid. Uroguanylin and plecanatide are both 16-amino acid peptides with optimal activity between pH 5 and 6.37 GC-C is expressed throughout the GI tract, but it has been proposed that by activating GC-C primarily in the small intestine (where the pH is in the 5– 6 range), elevation of secretions would be limited to the small intestine and not the large intestine, potentially limiting diarrhea as an adverse effect. Other than its activity limited to small intestine, researchers believe its mechanism of action is identical to linaclotide's. Plecanatide is metabolized completely within the GI tract, with plasma concentrations after an oral 3 mg dose being below limits of quantification.38
Plecanatide is taken once a day with or without food. Because of the risk of dehydration, this agent is contraindicated in patients younger than 6 years of age. Use is also contraindicated in those with known or suspected intestinal obstruction. In controlled trials, patients treated with plecanatide had a significant increase in CSBM compared with placebo. Patients also experience significantly better stool frequency and consistency compared with placebo.
The recommended daily dose of plecanatide is 3 mg; increasing the dose to 6 mg provides no additional benefit.38 The percentage of patients experiencing CSBM is significantly greater than placebo (3 mg, 21%; 6 mg, 19.5%, placebo, 10.2%; P < 0.001). This difference occurs as early as 1 week and persists through 12 weeks of treatment.39 Mild-to-moderate diarrhea is the most commonly reported adverse effect.
To date, no head-to-head, direct comparative studies of these agents have been completed. A meta-analysis confirmed that linaclotide was superior to placebo; however, this analysis found that bisacodyl may be superior to other drugs when evaluating the number of SBMs per week. Despite a large number of high-quality articles included, data from this analysis should be interpreted cautiously. Few randomized controlled trials were included, endpoints were different and were grouped by categories, treatment durations varied, and bisacodyl was often a rescue medication.40 Direct comparator studies are needed to determine if any clinical differences exist among these agents.
Case Study
Susan’s insurance will no longer cover lubiprostone but will cover either linaclotide or plecanatide. Susan states she still only has 3 or 4 CSBMs a week and the consistency of her stool is still somewhat hard. Between linaclotide and plecanatide, which drug would potentially be better for Susan to try?
Class-Wide Safety Concerns
Because of the intestinal secretagogues’ limited absorption, GI adverse effects are the primary concern; diarrhea is the most prominent concern. Clinicians must counsel patients to take these drugs properly to avoid or reduce incidence of nausea, vomiting, or diarrhea. While most adverse effects are mild to moderate in nature, severe adverse effects could lead to dehydration.
Because of the risk of dehydration, linaclotide and plecanatide are contraindicated in pediatric patients younger than 6 years of age. These drugs have not been fully studied in patients younger than 18 years of age and should be avoided in this population; additionally, lubiprostone is only indicated for adult women (older than 18 years).33,41,42
Clinicians should evaluate patients for GI obstructions; those with known or suspected obstructions should avoid use of these agents.33,41,42
CONCLUSION
CIC is the most common chronic GI disorder worldwide and affects almost 20% of patients. While anyone may be affected, females, patients older than 65, and those with less healthy lifestyles are at higher risk. Diagnosis of CIC is based upon the Rome IV diagnostic criteria. These criteria evaluate a number of symptoms such as number of bowel movements per week, stool consistency, and straining. Recent evidence supports the notion that CIC is on a disease spectrum with IBS and that patients may fluctuate between the two.
Once causes of constipation have been evaluated and ruled out, CIC should be differentiated from IBS. The hallmark symptoms of IBS (persistent abdominal pain and distention) are important in making this diagnostic distinction. While patients with CIC may present with these abdominal symptoms, they are not persistently present as they are with IBS. Patients with CIC frequently complain of straining, hard stools, bloating/discomfort, infrequent bowel movements, and the feeling that the bowel movement is incomplete. The BSFS is the standard assessment tool to determine stool consistency.
The primary goal of CIC treatment is to improve a patient’s bowel habits. Nonprescription fiber supplements and laxatives are key components of treatment. Diet and exercise are not well studied in CIC but should be encouraged as part of a healthy lifestyle. Patients using fiber supplements should select soluble fibers such as psyllium to reduce the incidence of cramping, bloating, and flatulence. Polyethylene glycol without electrolytes is preferred as it is more palatable than polyethylene glycol with electrolytes. For patients requiring long-term laxative therapy, non,timulant laxatives are preferred, as patients experience less diarrhea and abdominal distention than they do with stimulant laxatives.
Current prescription therapies include linaclotide, lubiprostone, and plecanatide. Each of these agents have been proven superior to placebo and have similar treatment outcomes. Differences primarily exist between their mechanisms and pharmacokinetic profiles. Linaclotide and plecanatide are contraindicated in patients younger than 6 years old because of the risk of dehydration, while lubiprostone is not recommended in patients younger than 18 years of age.
Diarrhea is the most common adverse effect associated with these 2 medications. When starting lubiprostone, patients may experience nausea. This can be lessened by taking with food and water, and the incidence greatly is greatly reduced after the first 5 days of treatment. Additionally, patients need to be counseled on the possibility of dyspnea within the first hour after taking their first dose. If this occurs, it should resolve within 3 hours. If dyspnea occurs with subsequent dosing, patients are encouraged to contact their health care provider. Most patients will require combination therapy with nonprescription laxatives, fiber supplements, and a prescription agent.
Multiple agents are in being studied in phase III clinical trials for the treatment of CIC. Prucalopride, naronapride, and velusetrag are selective 5-HT4 receptor agonists that have collectively been found to increase SBMs. These agents are thought to have little activity at the 5-HT1 and 5-HT2 receptors implicated previously in cardiotoxicity. Tenapanor, a NHE3-sodium transporter inhibitor, increases intestinal fluid volume thereby increasing frequency of BMs. Elobixibat, an ileal bile acid transporter inhibitor, also creates an osmotic effect by preventing the absorption of bile acids, which results in water being drawn into the intestinal lumen. Relamorelin, a ghrelin analog, increases gastric mobility and has been shown to increase appetite. As this agent is currently being studied primarily for diabetic gastroparesis, it remains to be seen what benefit it may have for patients with CIC.
Evaluation of patients with constipation must include a thorough history and assessment of symptoms. Patients should be encouraged to incorporate healthy habits, such as high-fiber diets and exercise, into their daily routines. Pharmacists should be prepared to help patients with nonprescription product selection. They also must provide counseling on prescription products so that patients fully understand administration instructions, potential adverse effects, and what benefits to expect from treatment.
REFERENCES
- Choung RS, Locke GR 3rd, Schleck CD, Zinsmeister AR, Talley JN. Cumulative
incidence of chronic constipation: a population-based study 1988-2003. Aliment
Pharmacol Ther. 2007;26(11-12):1521-1528.
- Suares NC, Ford AC. Prevalence of, and risk factors for, chronic idiopathic
constipation in the community: systematic review and meta-analysis. Am J Gastroenterol. 2011;106(9):1582-1591.
- Nellesen D, Yee K, Chawla A, Lewis BE, Carson RT. A systematic review of the
economic and humanistic burden of illness in irritable bowel syndrome and chronic
constipation. J Manag Care Pharm. 2013;19(9):755-764.
- Lacy BE, Mearin F, Chang L, Chey WD, Lembo AJ, Simren M, Spiller R. Bowel
Disorders. Gastroenterology. 2016;150(6):1393-1407.
- Rao SS, Rattanakovit K Patcharatrakul T. Diagnosis and management of chronic
constipation in adults. Nat Rev Gastroenterol Hepatol. 2016;13(5):295-305.
- Johanson JF, Kralstein J. Chronic constipation: a survey of the patient
perspective. Aliment Pharmacol Ther. 2007;25(5):599-608.
- O’Donnell LJ, Virjee J, Heaton KW. Detection of pseudodiarrhoea by simple
clinical assessment of intestinal transit rate. BMJ. 1990:300(6722):439-440.
- Longstreth GF, Thompson WG, Chey WD et al. Functional bowel disorders.
Gastroenterology 2006;130:1480-1491.
- Dukas L, Willett WC, Giovannucci EL. Association between physical activity,
fiber intake and other lifestyle variables and constipation in a study of women. Am J
Gastroenterology. 2003;9(5)8:1790-1796.
- De Schryver AM, Keulemans YC, Peters HP, et al. Effects of regular physical
activity on defecation pattern in middle-aged patients complaining of chronic
constipation. Scand J Gastroenterol. 2005;40(4):422–429.
- Ford AC, Moayyedi P, Lacy BE et al. American College of Gastroenterology
monograph on the management of irritable bowel syndrome and chronic idiopathic
constipation. Am J Gastroenterol. 2014;109 Suppl 1:S2-S26.
- Christodoulides S, Dimidi E, Fragkos KC, et al. Systematic review with meta-analysis: effect of fibre supplementation on chronic idiopathic constipation in adults. Aliment Pharmacol Ther. 2016;44(2):103-116.
- Paré P, Fedorak RN. Systematic review of stimulant and nonstimulant laxatives
for the treatment of functional constipation. Can J Gastroenterol Hepatol. 2014;28(10):549-557.
- Tack J, Camilleri M, Chang L, et al. Systematic review: cardiovascular safety
profile of 5-HT4 agonists developed for gastrointestinal disorders. Aliment Pharmacol
Ther. 2012;35(7):745-767.
- Briejer MR, Bosmans JP, Van Daele P, et al. The in vitro pharmacological profile
of prucalopride, a novel enterokinetic compound. Eur J Pharmacol. 2001;423(1):71-83.
- Shin A, Camilleri M, Kolar G, et al. Systematic review with meta-analysis: highly
selective 5-HT4 agonists (prucalopride, velusetrag or naronapride) in chronic
constipation. Aliment Pharmacol Ther. 2014;39(3):239-253.
- Quigley EM, Vandeplassche L, Kerstens R, Ausma J. Clinical trial: the efficacy,
impact on quality of life, and safety and tolerability of prucalopride in severe chronic
constipation—a 12-week, randomized, double-blind, placebo-controlled study. Aliment
Pharmacol Ther. 2009;29(3):315-328.
- Palme M, Milner PG, Bandman O, Ziola M, Canafax DM. A novel
gastrointestinal prokinetic, ATI-7505, increased spontaneous bowel movements (SMMs)
in a phase II, randomized, placebo-controlled study of patients with chronic idiopathic
constipation (CIC). Gastroenterology. 2010;138:S128-S129.
- ClinicalTrials.gov Registry, 2017. Velusetrag.
https://clinicaltrials.gov/ct2/results?cond=&term=Velusetrag&cntry1=&state1=&recrs=.
Accessed December 14, 2017.
- Goldberg M, Li Y-P, Johanson JF, Mangel AW, Kitt M, Beattie DT, Kersey K,
Daniels O. Clinical trial: the efficacy and tolerability of velusetrag, a selective 5-HT4 agonist with high intrinsic activity, in chronic idiopathic constipation—a 4-week,
randomized, double-blind, placebo-controlled, dose-response study. Aliment Pharmacol
Ther. 2010;32:1102-1112.
- Spencer AG, Labonte ED, Rosenbaum DP, et al. Intestinal inhibition of the
Na+/H+ exchanger 3 prevents cardiorenal damage in rats and inhibits Na+ ptake in
humans. Sci Transl Med. 2014;6(227):227ra36.
- Chey WD, Lembo AJ, Rosenbaum DP. Tenapanor treatment of patients with
constipation-predominant irritable bowel syndrome: a phase 2, randomized, placebo-controlled efficacy and safety trial. Am J Gastroenterol. 2017;112:763-774.
- Nakajima A, Seki M, Taniguchi S. Determining an optimal clinical dose of
elobixibat, a novel inhibitor of ileal bile acid transporter, in Japanese patients with
chronic constipation: a phase II, multicenter, double-blind, placebo-controlled
randomized clinical trial. J Gastroenterol. 2017; doi:10.1007/s00535-017-1383-5. [Epub
ahead of print.]
- Camilleri M, Acosta A. Relamorelin: a novel gastrocolokinetic synthetic Ghrelin
agonist. Neurogastroenterol Motil. 2015;27(3):324-332.
- Acosta A, Camilleri M, Kolar G, et al. Relamorelin relieves constipation and
accelerates colonic transit in a phase 2, placebo-controlled, randomized trial. Clin
Gastroenterol Hepatol. 2015;13(13):2312-2319.
- Chedid V, Camilleri M. Relamorelin for the treatment of gastrointestinal motility
disorders. Exp Opin Investig Drugs. 2017;26(10):1189-1197.
- Camilleri M, Murray JA. Diarrhea and Constipation. In: Kasper D, Fauci A,
Hauser S, Longo D, Jameson J, Loscalzo J. eds. Harrison’s Principles of Internal
Medicine, 19e. New York, NY: McGraw-Hill;
2014. http://accessmedicine.mhmedical.com.ezproxy.samford.edu/content.aspx?bookid=1130§ionid=79726207. Accessed November 02, 2017.
- Fabel PH, Shealy KM. Diarrhea, Constipation, and Irritable Bowel Syndrome In: DiPiro JT, Talbert RL, Yee GC, Matzke GR, Wells BG, Posey LM, eds. Pharmacotherapy: A Pathophysiologic Approach, 10e. New York, NY: McGraw-Hill;
§ionid=146059459. Accessed November 02, 2017.
- Thomas RH, Luthin DR. Current and emerging treatments for irritable bowel
syndrome with constipation and chronic idiopathic constipation: focus on prosecretory
agents. Pharmacotherapy. 2015;35(6):613-630.
- Christie J, Shroff S, Shahnavaz N, et al. A randomized, double-blind, placebo-controlled trial to examine the effectiveness of lubiprostone on constipation symptoms
and colon transit time in diabetic patients. Am J Gastroenterol. 2017;112(2):356-364.
- Li F, Fu T, Tong WD, et al. Lubiprostone is effective in the treatment of chronic
idiopathic constipation and irritable bowel syndrome: A systematic review and meta-analysis of randomized controlled trials. Mayo Clin Proc. 2016;91(4):456-458.
- Cryer B, Drossman DA, Chey WD, et al. Analysis of Nausea in Clinical Studies
of Lubiprostone for the Treatment of Constipation Disorders. Dig Dis Sci. 2017;62(12):3568-3578.
- Amitiza® [package insert]. Sucampo Pharmaceuticals, Inc., Bethesda, MD; 2012.
- Chang L, Lembo AJ, Lavins BJ, et al. The impact of abdominal pain on global
measures in patients with chronic idiopathic constipation, before and after treatment with
linaclotide: a pooled analysis of two randomised, double-blind, placebo-controlled, phase
3 trials. Aliment Pharmacol Ther. 2014;40(11-12):1302-1312.
- Lacy BE, Schey R, Shiff SJ, et al. Linaclotide in chronic idiopathic constipation
patients with moderate to severe abdominal bloating: A randomized, controlled trial. PLoS One. 2015;10(7):e0134349.
- Koliani-Pace J, Lacy BE. Update on the management of chronic constipation. Curr Treat Option Gastroenterol. 2017;15(1):126-134.
- Brancale A, Shailubhai K, Ferla S, et al. Therapeutically targeting guanylate
cyclase C: computational modeling of plecanatide, a uroguanylin analog. Pharmacol Res
Perspect. 2017;5(2):e00295.
- Al-Salama ZT, Syed YY. Plecanatide: first global approval. Drugs. 2017;77(5):593-598.
- Miner PB, Koltun WD, Wiener GJ, et al. A randomized phase III clinical trial of
plecanatide, a uroguanylin analog, in patients with chronic idiopathic constipation. Am J
Gastroenterol. 2017;112(4):613–621.
- Nelson AD, Camilleri M, Chirapongsathorn S, et al. Comparison of efficacy of
pharmacological treatments for chronic idiopathic constipation: a systematic review and
network meta-analysis. Gut. 2017;66(9):1611-1622.
- Linzess® [package insert]. Ironwood Pharmaceuticals, Inc., Cambridge, MA;
2017.
- Trulance® [package insert]. Synergy Pharmaceuticals, Inc., New York, NY;
2017.
Back Top