
Expired activity
Please go to the PowerPak
homepage and select a course.
Module 8. Diabetes and Nutrition 101
Nutrition is one of the most controversial health topics, with opinions about what constitutes a healthy diet ranging from one extreme (e.g., low carbohydrate) to the other (e.g., low fat). Diet is a major consideration for those managing diabetes and, while carbohydrates have garnered the most interest related to glycemic control, other dietary components are likely very important.
Given the controversies related to nutrition, even some of the most reputable organizations, such as the American Diabetes Association (ADA), have chosen to refrain from giving specific dietary guidelines to people with diabetes, stating in their Standards of Care that, “there is not a one-size-fits-all eating pattern for individuals with diabetes, and meal planning should be indivdiualized”1 The ADA further states that studies examining the ideal amount of carbohydrate intake for people with diabetes are inconclusive. However, they do acknowledge that “monitoring carbohydrate intake and considering the blood glucose response to dietary carbohydrate are key” for improving postprandial control. The United States Department of Agriculture (USDA) MyPlate guide to eating is the most current food guide pyramid (i.e., accessible at ChooseMyPlate.gov). MyPlate provides nutritional guidance to the American population as a whole; but, it is not necessarily the key to eating as a means to control blood glucose levels in people with diabetes or prediabetes. MyPlate recommends that half of an individual’s daily plate of food consist of fruits and vegetables. While such dietary intake will likely increase the intake of nutrients and phytochemicals,2 produce varies widely in its nutritional content and, therefore, in its glycemic impact on people with diabetes.3
Many people with type 2 diabetes mellitus (T2D) are counseled to lose weight to help manage or potentially reverse diabetes or pre-diabetes. Weight loss may be a useful goal for people with T2D who are overweight, but it may have to exceed 5% in order to impact blood glucose control.4,5 Sustaining a weight loss of as little as 5% to 7% of body weight can lead to a decrease in insulin resistance and improvement in blood glucose control and, therefore, allows for a reduction in the amount of medication taken.6 Along the same lines, even preventing excessive weight gain in those with type 1 diabetes mellitus (T1D) can help keep insulin action high and insulin needs lower by preventing or reducing insulin resistance.7 While the nutrition focus in this module is on the benefits of balancing carbohydrates, fats, and protein in the diet to control blood glucose levels, improvements in body weight will likely also result from a healthier diet and other lifestyle improvements.
The ADA lists the following as goals for nutrition therapy for adults with diabetes:1
- To promote and support healthful eating patterns, emphasizing a variety of nutrient-dense foods in appropriate portion sizes, to improve overall health and:
- Achieve and maintain body weight goals
- Attain individualized glycemic, blood pressure, and lipid goals
- Delay or prevent the complications of diabetes
- To address individual nutrition needs based on personal and cultural preferences, health literacy and numeracy, access to healthful foods, willingness and ability to make behavioral changes, and barriers to change
- To maintain the pleasure of eating by providing nonjudgmental messages about food choices
- To provide an individual with diabetes the practical tools for developing healthy eating patterns rather than focusing on individual macronutrients, micronutrients, or single foods
WHAT CONSTITUTES A HEALTHY DIET FOR PEOPLE WITH DIABETES?
Carbohydrates, fats, and proteins are the dietary macronutrients that provide energy for activity and routine body functioning, although each of these nutrients has a different primary role. Protein helps to build muscle and other bodily structures, while fat is important as a source of stored energy and contributes to the health of the brain, nerves, hair, skin, and nails. Carbohydrate is a major fuel source for the body, especially during physical activity, and is the primary supplier of energy for the brain, nerves, and muscles.
The quality of dietary fats and carbohydrates consumed is more crucial than is the quantity of these macronutrients. Diets rich in whole grains, fruits, vegetables, legumes, and nuts; moderate in alcohol consumption; and lower in refined grains, red or processed meats, and sugar-sweetened beverages have been shown to reduce the risk of diabetes and improve glycemic control and blood lipids in patients with diabetes.8 There is currently insufficient evidence to suggest that any particular diet is superior for treating overweight and obese patients with T2D; although the Mediterranean, vegan, and low-glycemic index diets appear to be promising.9 When overall diet quality is emphasized, several dietary patterns, such as Mediterranean, low-glycemic index, low carbohydrate intake, and vegetarian diets, can be tailored to personal and cultural food preferences and appropriate calorie needs for weight control and diabetes prevention and management.10-12
Regardless of a patient’s overall dietary pattern, it may be useful to check blood glucose levels before and after meals to learn how foods affect each individual, particularly for those ingesting a lot of carbohydrates (e.g., such as potatoes, bread, rice, and pasta). People should focus on keeping portion sizes reasonable and manage blood glucose levels by providing a good balance of carbohydrates, fats, and protein. Everyone, including all people with diabetes, will benefit from an appropriate balance of these 3 macronutrients.
|
Sidebar: Does Your Plate Look Like This?
Create Your Plate (see Figure 1) is a tool used to assist patients with managing diabetes and losing weight. It encourages individuals to choose more non-starchy vegetables and smaller portions of starchy foods and protein. It is a simply to use strategy and has an online interactive tool including examples for each food category.
Figure 1. Create Your Plate!
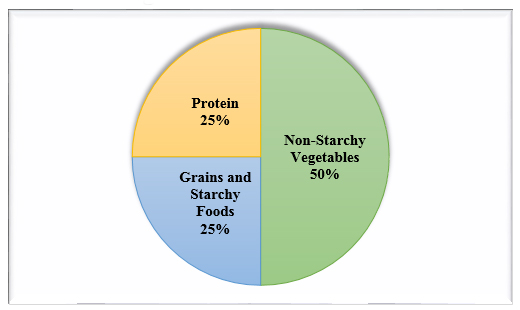
- Using your dinner plate, put a line down the middle of the plate. Then on one side, cut it again so you will have three sections on your plate.
- Fill the largest section with non-starchy vegetables.
- Now in one of the small sections, put grains and starchy foods.
- And then in the other small section, put your protein.
- Add a serving of fruit, a serving of dairy or both as your meal plan allows.
- Choose healthy fats in small amounts. For cooking, use oils. For salads, some healthy additions are nuts, seeds, avocado and vinaigrettes.
- To complete your meal, add a low-calorie drink like water, unsweetened tea or coffee.
Adapted from CreateYour Plate (http://www.diabetes.org/food-and-fitness/food/planning-meals/create-your-plate/).
|
Carbohydrate Intake
Carbohydrates have the greatest impact on the amount of glucose in the blood because they are converted to glucose relatively quickly. Many people with diabetes try to avoid or limit their intake of carbohydrates as a way to maintain healthy blood glucose levels, but the human body requires the fiber found in plant foods. Carbohydrates are also the body’s first choice for fuel during many physical activities; so, not having enough in the diet may limit a person’s ability to exercise optimally.
Many people with diabetes count the grams of carbohydrates in foods to help them control their blood glucose levels, and others choose carbohydrates based on their glycemic index (i.e., how rapidly the food item raises blood glucose levels).13 The exact amount of carbohydrates a person with diabetes should ingest varies based on physical activity levels, medications used, and overall insulin action. Starches and sugars ideally should be limited, but not fiber and non-starchy vegetables, such as salad greens, peppers, tomatoes, green beans, carrots, cauliflower, and onions.
Fiber Intake: Fiber includes all indigestible polysaccharides (i.e., a type of complex carbohydrate), including the natural ones in foods and others that are extracted or isolated from foods or made synthetically (e.g., Metamucil fiber supplement).14 Soluble fiber, which is found in oatmeal, legumes, seeds, fruits (e.g., apples, bananas, citrus fruits), and vegetables, dissolves in water, is partially metabolized in the large intestine by health-promoting bacteria, and helps lower blood cholesterol. Oats in particular may have a strong anti-inflammatory effect by increasing these healthful bacteria in the intestinal tract.15 An insoluble form of fiber is found in carrots, celery, and the skins of corn kernels; fruit peels, cores, and seeds; brown rice; and whole grains. Acting as roughage, most fiber passes through the human digestive system without being fully digested and ensures regular bowel movements. Since it resists acids and digestive enzymes in the stomach, fiber cannot be fully digested and does not add calories to the diet. The ADA specifically recommends that “carbohydrate intake should emphasize nutrient-dense carbohydrate sources that are high in fiber, including vegetables, fruits, legumes, whole grains, as well as dairy products.”1
In addition to those previously mentioned, dietary fiber has many other health and metabolic benefits.14 For instance, a high-fiber diet may help reduce the chances of developing heart disease, diabetes, obesity, strokes, colorectal and other types of cancer, diverticulosis, and hemorrhoids.14 Regular intake of sufficient fiber has additionally been associated with lower all-cause mortality in people with diabetes.16,17 Fiber adds bulk and aids in portion control because it generally slows down the rate at which food empties from the stomach, makes people feel full longer, and prevents excessive eating and weight gain. From a diabetes and a personal health standpoint, dietary fiber may reduce blood glucose and cholesterol, all while slowing the digestion of carbohydrates to glucose, thereby keeping blood glucose levels more stable.
Current research is focusing on the role of the gut microbiome—the bacteria that reside in the intestinal tract—on human health and disease. The human body hosts 100 trillion, mostly benign bacteria, which help digest food, program the immune system, prevent infection, and even influence mood and behavior. The bacteria living on and in us make up an ecosystem that likely plays a role in many conditions that genes and environmental factors alone fail to explain, including obesity, autism, depression, asthma, irritable bowel syndrome, and even cancer.18
In fact, it is very possible that the type of bacteria people have in their gut has a huge impact on whether they gain weight or stay slim, get diabetes or avoid it, and develop other chronic diseases or stay healthier.18 Although this research is ongoing, it is clear is that fiber enhances the gut’s abundance of the good bacteria that reduce inflammation. For no other reason, patients with diabetes (and other metabolic health conditions) should consume recommended levels of fiber as to keep their health-promoting gut bacteria thriving and abundant.
A good target is at least 20 to 35 grams of dietary fiber per day. Fiber is found only in plant-based foods, such as oats, oat bran, ground flaxseed, beans, fruits, wheat bran, apple peels, and most vegetables. Instead of trying to eat a certain amount, it may be easier to simply eat more nutritious types of plants, fruits, and vegetables, in addition to whole grains, legumes, nuts, and seeds.
Fat Intake
Diabetes can result in unhealthy changes in blood fats. In addition, elevated levels of triglycerides, which can result from eating highly refined carbohydrates and less healthy types of cholesterol, plays a major role in stimulating the inflammatory process leading to the development of cardiovascular disease common to people with diabetes.20 Not every type of fat is bad, although the proposed health benefits attributed to various types of fats are still being hotly debated in the nutrition world. But, it has been proven that a high intake of certain types of fat, as well as the intake of refined carbohydrates, can contribute to the development of insulin resistance and negative changes in blood fats.21
Eat Fewer Trans Fats and Processed Fats: Trans fats are created by manufacturers when they hydrogenate or partially hydrogenate liquid oils to alter their texture. Consumption of trans fats found in hydrogenated oils contributes to insulin resistance and makes it harder to control blood glucose and cholesterol levels. Found most abundantly in processed foods, crackers, cookies, and baked goods, trans fats may be disguised as monoglycerides and diglycerides, stearate, palmitate, lard, vegetable shortening, and hydrogenated or partially hydrogenated oils. The minimal amount of trans fats found in natural sources (e.g., cheese), however, are not considered as unhealthy as the manufactured trans fats.22 The ADA specifically recommends that diets rich in monounsaturated and polyunsaturated fats (such as a Mediterranean-style diet) may be considered to improve glucose metabolism and lower cardiovascular disease risk.1
|
Sidebar: Mediterranean-style diet
So what is considered a “Mediterranean-style diet”? A recently published consensus document from the ADA describes a Mediterranean-style diet as a diet that:23
“Emphasizes plant-based food (vegetables, beans, nuts and seeds, fruits and whole intact grains); fish and other seafood; olive oil as the principle source of dietary fat; dairy products (mainly yogurt and cheese) in low to moderate amounts; typically fewer than 4 eggs/week; red meat in low frequency and amounts; wine in low to moderate amounts; and concentrated sugars or honey rarely.”
The ADA consensus report additionally states that Mediterranean-style diets have been shown to potentially reduce the risk of diabetes, decrease A1C, lower triglyceride levels, and reduce the risk of major cardiovascular events.
|
Highly processed meats (e.g., bacon, sausage, and lunch meats) are also likely bad for health because of the preservatives added. For example, eating even one fast food meal high in both manufactured trans fats and highly processed fats can interrupt the normal flow of blood through arteries and veins for hours afterward and make the body’s response to insulin sluggish as well. Conversely, eating a high-fat breakfast that contains mostly a good fat, such as olive oil, allows blood glucose and insulin levels to stay lower.24 A high intake of highly processed meat has been associated with a higher risk of T2D.25,26
Eat More Omega fats and Healthy Plant Fats: The following 2 dietary polyunsaturated fats are essential to good health: omega-3 and omega-6 fats. Both are important to include in a healthy diet, particularly for people with diabetes whose nutrition is even more important to preserve their long-term health. ADA states that “eating foods rich in long-chain n-3 fatty acids, such as fatty fish and nuts and seeds, is recommended to prevent or treat cardiovascular disease. 1 Omega-3 fats are abundant in dark green, leafy vegetables (e.g., dark-colored lettuce, spinach, kale, turnip greens), canola oil, flaxseed oil, soy, some nuts (e.g., walnuts), fish, and fish oils.
Only fish and fish oils contain larger amounts of the 2 omega-3 fats called docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA) that are critical for brain and nerve function, cardiovascular health, and more. Plant foods contain mainly the essential omega-3 fat called alpha-linolenic acid (ALA), which may be converted, by the body, into DHA and EPA if intake is low.
Omega-6 fats are abundant in the corn, sunflower, peanut, and soy oils used to make food products, such as margarine, salad dressing, and cooking oils, and they may actually help lower inflammation.27 A high vegetable fat intake may decrease type 2 diabetes risk for women.28 While foods rich in long-chain n-3 fatty acids are recommended, evidence does not currently support a beneficial role for routine use of n-3 dietary supplements.1
Diets high in certain types of fat, such as the plant-based fats found naturally in avocados, may actually improve insulin action. Even tropical oils that are saturated and minimally processed are considered healthier options (e.g., coconut). Unnaturally low-fat diets can cause the liver to produce more bad cholesterol, especially if people replace fat with refined carbohydrates.21
HEALTHINESS OF FAT IN RED MEAT, DAIRY, EGGS, AND NUTS
The topic of red meat being a health concern has been accepted since the 1960s. Studies have shown that the likely culprit in red meat is carnitine, and gut microbes that break down this compound into harmful byproducts such as TAMO that has been associated with atherosclerosis risk.25 The old adage remains true for now, the less red meat in your diet, the better. Do not despair though, many healthier choices are available, including fish, nuts, legumes, fruits, and vegetables. As a method of reducing calorie intake, it is safe to suggest or recommend consumption of the low-calorie or low-fat versions of dairy products, such as cheese and milk.29 Also, diets rich in the monounsaturated fats found in olive oil, canola oil, and nuts and seeds are heart healthy and do not necessarily promote weight gain. Actually, if someone is following a weight loss diet and eats a handful of almonds or other nuts daily, he or she is likely to lose more weight than eating the same number of calories without the nuts.30
Blood cholesterol levels should decrease as people eliminate trans fats and other processed fats from their diets. Everyone must have a certain amount of cholesterol, which is a waxy, fat-like substance important in cell and hormone composition; the liver will excrete cholesterol as needed. Cholesterol is found in all animal products, including meat, poultry, dairy, eggs, and all types of fish, but not in plants. More recent studies indicate that the cholesterol found in eggs may not be as detrimental as once thought; the cholesterol in egg yolks has not been proven to raise blood cholesterol levels or increase the risk for cardiovascular disease.
Protein Intake
Protein has a minimal and immediate effect on blood glucose levels and it aids in the sensation of fullness. In fact, low-protein meal plans are associated with increased hunger; therefore, eating more lean protein along with healthy fats may reduce appetite and help people achieve and maintain a lower calorie intake. Adequate intake of protein also helps to maintain lean body mass, so it is beneficial for those who lose weight on a diet or gain more muscle mass from exercising, and eating enough protein is important for aging well.
Most foods with a significant amount of protein have a lower glycemic effect because protein is metabolized more slowly than carbohydrates, usually within 3 to 4 hours. In patients with T2D, an increase in protein intake does not increase plasma glucose; but it will increase the insulin response and leads to lower A1C levels.31 In fact, consuming as much as 30% to 40% of calories as protein, with a lower intake of carbohydrates and fats, may assist with diabetes control, weight loss, and weight maintenance. However, a high intake of protein from processed meats actually increases diabetes risk.26 Advise patients to choose high-quality sources of protein, such as lean meats and poultry, soy products, legumes, and fish. Moreover, a diet rich in soy protein appears to have a lasting beneficial effect for people with T2D because it lowers fasting blood glucose levels, blood fats, C-reactive protein (an indicator of inflammation), and markers of kidney disease.
In the past, protein intake has been blamed for declines in kidney function and frequently restricted in the diets of people with diabetes for that reason. However, the relationship between protein intake as grams per kilogram of body weight and albumin excretion rate is very weak, except for patients with hypertension and, particularly, for those with uncontrolled diabetes. Currently, a protein intake of approximately 0.8 g/kg per day (the recommended daily allowance) should be recommended for patients with diabetes and chronic kidney disease.32
CARBOHYDRATE COUNTING VERSUS CALORIE COUNTING
Estimating how much insulin is needed to cover meals and snacks is frequently difficult. Many people with diabetes have been taught to count carbohydrates; so, they try to estimate the actual amount of carbohydrates, in grams, ingested and give themselves specific doses of mealtime insulin based on an insulin-to-carbohydrate ratio that works for them. Although carbohydrate counting has been shown to improve glycemic control, it is far from an exact science33 and a nearly impossible task for individuals with below average health literacy or numeracy skills.1 When weight loss occurs as the successful outcome of a Mediterranean, vegan, or low-glycemic index diet, greater improvements in A1C levels can be seen as compared with more standard dietary patterns followed by adults with T2D who are overweight.9
More recently, it has been recognized that estimating protein intake for individuals with T1D is also important for controlling spikes in blood glucose after meals—rather than only estimating and accounting for carbohydrate intake—because some of the protein is converted into glucose (albeit more slowly than carbohydrates).34 Protein takes 3 to 4 hours to be fully metabolized and some can be converted into blood glucose when digested; therefore, a higher protein intake can contribute to higher blood glucose levels later on, mostly for people who have to inject or pump appropriate amounts of insulin and are using rapid-acting insulin analogues.
To complicate matters, eating a meal with more fat in it has also been shown to increase insulin needs for those with T1D, even when the carbohydrate content is held constant, suggesting that alternative insulin dosing algorithms are needed for higher-fat meals.35 Fat may slow down, slightly, the absorption of carbohydrates in the meal, but it does not change the overall blood glucose peak.36 Vegan meals have been suggested as a healthy alternative for people with T2D, but their higher carbohydrate content may result in greater postprandial increases in blood glucose compared with meat-based dietary patterns.3
Thus, all calories can potentially raise blood glucose at some point, not just those coming from carbohydrates.37,38 This critical point was aptly made in a recent review of all studies done to date, which reported that high-fat and high-protein meals both require more total insulin than a meal with less fat or protein and an identical carbohydrate content.39 If a person with diabetes is unable to release enough insulin to cover blood glucose increases arising from the consumption of all types of macronutrients, he or she will need to take exogenous doses of insulin to compensate.
Several terms have been used to categorize and/or quantify the types of carbohydrates consumed and the impact that carbohydrates consumed have on blood glucose:
Glycemic Index (GI)
How rapidly a carbohydrate is digested affects insulin responses and the ability to control blood glucose, as reflected by its glycemic index (GI). The more rapidly a food is broken down, the faster the carbohydrate is turned into blood glucose.13
Glycemic Load (GL)
Glycemic load (GL) is a measure of both GI value and total carbohydrate intake in a typical serving. A GL of 20 or more is considered high, 11 to 19 is considered medium, and 10 or less is considered low. 40
Food Insulin Index (FII)
Some of the same researchers who developed the GI have since attempted to systematically rate insulin responses to common foods, instead of simply postprandial glucose spikes, the result being the food insulin index (FII), an alternate measurement that can be used in place of counting GI or carbohydrates.41
The use of GI, GL and FII continues to be of interest to rank carbohydrate foods according to their effects on glycemia, yet a recently published ADA consensus report notes some uncertainly about the use of these tools in general clinical care. 23 This uncertainty stems from two systematic reviews of GI and GU that reported no significant impact of use in individuals with diabetes or those at risk for diabetes on A1C, with mixed results on fasting glucose.42,43
USE OF SUGAR, SUGAR ALCOHOLS, AND OTHER SUGAR SUBSTITUTES
Foods that are higher in fiber are also, on the whole, lower in added sugars, fat, and calories. White sugar has only a medium-GI value and a low GL, but the health impact of eating a lot of white sugar and other refined carbohydrates is not trivial, particularly given their lack of essential nutrients and high calorie content. While it is not necessary to give up refined sugars completely, limiting their intake will help with glycemic control and cholesterol levels as well.
One of the easiest ways to start lowering the sugar content of a person’s diet and improving its glycemic effect is to reduce or eliminate the intake of all regular soft drinks, fruit juice drinks, and sugar-sweetened iced tea or lemonade. Substitute sugary drinks with water, diet soft drinks (especially the non-caffeinated, non-cola varieties), or other artificially sweetened beverages. The ADA places emphasis on water intake.1
As for fructose, there is nothing inherently evil about this simple sugar naturally found in fruit, despite research that has suggested that high-fructose corn syrup in beverages leads to a fatty liver. More likely, it is an excess intake of calories that leads to such health issues, not fructose.44
Some products are touted as sugar free because they contain sugar alcohols, which are reduced-calorie sweeteners (i.e., usually about half the number of calories as sugar). Blood glucose responses to different sugar alcohols (e.g., sorbitol, xylitol, and lactitol) may vary; but, in general, they will have less of an impact on blood glucose levels than other carbohydrates because these types of sugars are not fully metabolized into calories. Although helpful for reducing calories and blood glucose, sugar alcohols are not completely calorie free and may cause a laxative effect in some people.
Finally, using sugar substitutes or other low-calorie sweeteners may help people reduce their calorie intake. They also reduce the intake of high-GI carbohydrates when used in place of sugar to sweeten coffee, tea, cereal, or fruit by adding sweetness without calories. Approved sugar substitutes include saccharin, aspartame, acesulfame potassium, sucralose, neotame, tagatose, and stevia, to name a few. All are considered safe to use and are recommended for people with diabetes by the American Diabetes Association. Sucralose (Splenda) is one of the most popular ones and has largely replaced aspartame (NutraSweet) in many products, but some people are sensitive to it and experience negative reactions like headaches or stomach upset. Newest to the market is Stevia, a sweetener and sugar substitute extracted from the leaves of the plant species Stevia rebaudiana found in South America. It is 200 times sweeter than sugar, but contains no calories and is a more natural product alternative.
The 2019 ADA Standards of Medical Care in Diabetes offer the following recommendations related to sugar-sweetened beverages and nonnutritive sweeteners:1
- People with diabetes and those at risk are advised to avoid sugar-sweetened beverages (including fruit juices) in order to control glycemia and weight and reduce their risk for cardiovascular disease and fatty liver and should minimize the consumption of foods with added sugar that have the capacity to displace healthier, more nutrient-dense food choices.
- The use of nonnutritive sweeteners may have the potential to reduce overall calorie and carbohydrate intake if substituted for caloric (sugar) sweeteners and without compensation by intake of additional calories for other food sources.
- For those who consume sugar-sweetened beverages regularly, a low-calorie or nonnutritive-sweetened beverage may serve as a short-term replacement strategy, but overall, people are encouraged to decrease both sweetened and nonnutritive-sweetened beverages and use other alternatives, with an emphasis on water intake.
MICRONUTRIENTS AND SUPPLEMENTS
A large number of supplements and nutrients are touted for their potential benefits in the management of diabetes and its complications. In the community setting, it is very common for pharmacy professionals to field questions about supplements and vitamins for this purpose. Unfortunately, there continues to be a lack of strong evidence of benefit from herbal products, vitamins, and minerals to help with glucose control in people with diabetes in the absence of an underlying deficiency.23
Vitamin B12 supplementation in people on metformin therapy, however, has gained recent attention. The ADA states that: “long-term use of metformin may be associated with biochemical vitamin B12 deficiency, and periodic measurement of vitamin B12 levels should be considered in metformin-treated patients, especially in those with anemia or peripheral neuropathy.”45 As such, vitamin B12 supplementation in people with T2D on metformin therapy will continue to increase.
What about other supplements and micronutrients? The ADA states that there is no clear evidence that dietary supplementation with vitamins, minerals (such as chromium and vitamin D), herbs, or spices (such as cinnamon or aloe vera) can improve outcomes in people with diabetes who do not have underlying deficiencies and they are not generally recommended for glycemic control. 1 Regardless, many people with diabetes use supplements and herbal products and should be asked about over-the-counter and herbal products to ensure safe and appropriate use.
ALCOHOL
Alcohol intake is another important matter when considering nutrition in people with diabetes. Moderate alcohol intake does not have major effects on long-term glucose control. 1 The primary considerations with alcohol consumption in people with diabetes are risk of hypoglycemia (particularly for people being treated with insulin or insulin secretagogue medications), weight gain, and hyperglycemia.23 The ADA recommends that women limit their consumption of alcohol to no more than 1 drink per day, and nor more than 2 drinks per day for men. A drink is defined as a 12-oz beer, a 5-oz glass of wine, or 1.5 oz of distilled spirits. For people being treated with insulin or insulin secretagogue medications, education and awareness regarding recognition and management of delayed hypoglycemia are warranted.
COFFEE AND CAFFEINE
Caffeine has no calories and it stimulates metabolism; so, it presents the following questions: Can people with diabetes have regular coffee with breakfast? Can people with diabetes drink diet colas, iced tea, and other caffeinated drinks? Evidence suggests caffeine can make the body more insulin resistant, rather than improving the chance of avoiding diabetes by drinking coffee, as earlier studies had claimed.46,47 In lean people, obese people, and people with T2D equally, caffeine ingestion in the amount equivalent to two to three 8-ounce cups of coffee a day (i.e., 5 mg per kg of body weight) reduces insulin action by about one-third and the caffeine-induced decrement is still present after as many as 3 months of moderate aerobic exercise (which usually increases insulin action).48
The effects of coffee drinking have been studied in people controlling T2D with diet, exercise, and oral medications only. Participants wearing a glucose monitor continuously for 72 hours revealed that 2 cups of coffee daily increased blood glucose levels by 8%.49 Caffeine intake also exaggerated the rise in their blood glucose after meals as follows: by 9% after breakfast, 15% after lunch, and 26% after dinner. People with T2D who had caffeine before doing an oral glucose tolerance test were also more insulin resistant.50
INTERPRETING FOOD LABELS AND DETERMINING PORTION SIZES
Food Labels
The FDA recently made regulatory changes to food labeling that will help consumers better understand the content of their food choices. The new Nutrition Facts label includes a new design to make it easier to understand calories and serving size. Historically, it has been difficult for consumers to understand the concept of what actually constitutes one serving. This will be highlighted on the new labeling. A percentage daily value of added sugars is also included in the new labeling, as well as the type of fat contained in a product, not just calories from fat. 51
Serving Size is always at the top of the nutrition facts label. The nutrition information provided is for the serving size that is stated on the label. Remember that the serving size on the label may not be the same as the portions that people usually eat. To determine the grams of carbohydrate, other macronutrients, or calories in a given product, be sure to check the serving size because the official serving sizes can be quite small as compared with how much people usually consume at one sitting.
For the control of blood glucose, people should focus on the grams of total carbohydrate rather than the grams of sugar listed in the indented list that follows (e.g., grams of dietary fiber, total sugars, etc.). Sugars and fiber are counted as part of the grams of total carbohydrate. If a food contains fiber, however, people should subtract the fiber grams from the total carbohydrate for a more accurate estimate of the carbohydrate content of a food because fiber is not digested—particularly if each serving contains 3 or more grams of fiber. If a food contains sugar alcohols, subtract one half of the grams of sugar alcohols listed on the label from the total carbohydrate content as they are not fully metabolized. Added Sugars, as a subcategory of Sugars has finally been added to food labels to make it easier for consumers to understand that there may be a health difference between something like the sugars naturally occurring in fruit (fructose) and the white sugars added to beverages and processed foods.
Manufacturers must list ingredients in the order of descending weight. In many products, refined sugar would be listed first; or it may be disguised as 4 or 5 different sweeteners that appear lower on the list. Look for sugar equivalents, such as sucrose, dextrose, high-fructose corn syrup, corn syrup, glucose, fructose, maltose, levulose, honey, brown sugar, and molasses in the ingredient list. They are all now included as part of the Added Sugars and Total Carbs.
Portion Control
Although it may not be accurate to designate any foodstuff as completely bad for health, some foods should be eaten in small quantities only. It is important to remember, however, that many people experience something referred to as portion distortion and become confused about what an appropriate portion size may be for a person of a specific weight and height. People tend to interpret the size of their meal, regardless of how big or small it is, to be an appropriate portion. By definition, a serving size is not the amount a person puts on his or her plate; rather, it is a specific amount of food, defined as cups, ounces, or pieces, whereas a portion is the amount of food that a person chooses to eat, which can be more or less than a serving. Standardized serving sizes are required to be listed on all food labels, but even these are currently being revised by the USDA.
|
Sidebar: Portion Versus Serving Sizes
- Many people think the portion in front of them is the appropriate portion size to eat, regardless of how big or small it actually is
- A serving size is a determined amount on a food label and may or may not be the correct portion size
- What is an appropriate portion size varies from person to person
|
Most people do not conceptualize portions very well; nor do they have a good sense of their hunger or satiety. For instance, researchers gave participants a lunch of macaroni and cheese every day and each day they were unknowingly served larger and larger portions of macaroni and cheese, leading them to eat more each day without realizing it. In another study, participants who ate from secretly refilling bowls were estimated to have eaten 73% more soup than controls; but, these participants reported feeling no more satisfied than those who ate less soup and fewer calories.
CONCLUSIONS
There is a lot of controversy regarding what constitutes a healthy diet, especially for those with diabetes. However, a balanced intake of carbohydrates, fats, and proteins; a severe reduction in the consumption of processed foods, refined sugars, and carbohydrates; combined with an increase in the amount of fiber consumed daily will likely improve glycemic control and the overall health of all individuals with or without diabetes. Counting carbohydrates may not be as useful as controlling overall calorie intake and choosing foods that require less insulin (as determined with the food insulin index), although use of the GI and GL can improve outcomes. Sugar substitutes are safe for people with diabetes and can help reduce both glucose spikes and calorie intake. It is also important to recognize an appropriate serving of food and realize that a perceived portion may not necessarily be the same as an appropriate serving. Overall, it is possible for people with diabetes to improve their overall glycemic control and health with appropriate changes to their diet.
| Counseling Tips for Pharmacists |
| Category |
Counseling Tips |
| General Diabetes Education |
- There is insufficient evidence to suggest that any particular diet is superior for treating overweight and obese patients with type 2 diabetes; but the Mediterranean, vegan, and low-glycemic index diets show promise.
- Diets rich in whole grains, fruits, vegetables, legumes, and nuts; moderate in alcohol consumption; and lower in refined grains, red or processed meats, and sugar-sweetened beverages have been shown to reduce the risk of diabetes and improve glycemic control and blood lipids in patients with diabetes.
- Carbohydrates have the greatest impact on the amount of glucose in the blood because they are converted to glucose relatively quickly.
- Carbohydrates are also the body's first choice for fuel during many physical activities; so, not having enough in the diet may limit a person's ability to exercise optimally.
- People with diabetes should eat plenty of fiber in their diet.
- People with diabetes should eat fewer trans fats and processed fats. Trans fats are created by manufacturers when they hydrogenate or partially hydrogenate liquid oils to alter their texture.
- People with diabetes should eat more omega fats and healthy plant fats. Omega-3 fats can be found in dark green, leafy vegetables, canola oil, flaxseed oil, soy, some nuts, fish, and fish oils. Omega-6 fats are abundant in the corn, sunflower, peanut, and soy oils used to make food products, such as margarine, salad dressing, and cooking oils.
- Protein has a minimal and immediate effect on blood glucose levels and it aids in the sensation of fullness.
- All calories can potentially raise blood glucose at some point, not just those coming from carbohydrates.
- One of the easiest ways to start lowering the sugar content of a person's diet and improving its glycemic effect is to reduce or eliminate the intake of all regular soft drinks, fruit juice drinks, and sugar-sweetened iced tea or lemonade. Whenever possible drink water.
|
REFERENCES
- American Diabetes Association. 5. Lifestyle management: Standards of Medical Care in Diabetes - 2019. Diabetes Care. 2019;42(Suppl. 1):S46-S60.
- Slavin JL, Lloyd B. Health benefits of fruits and vegetables. Advances in nutrition.Bethesda, Md. 2012;3:506-516.
- Belinova L, Kahleova H, Malinska H, et al. Differential acute postprandial effects of processed meat and isocaloric vegan meals on the gastrointestinal hormone response in subjects suffering from type 2 diabetes and healthy controls: a randomized crossover study. PLoS One. 2014;9:e107561.
- Franz MJ, Boucher JL, Rutten-Ramos S, VanWormer JJ. Lifestyle weight-loss intervention outcomes in overweight and obese adults with type 2 diabetes: a systematic review and meta-analysis of randomized clinical trials. J Acad Nutr Diet. 2015;115:1447-1463.
- Lean ME, Leslie WS, Barnes AC, et al. Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. Lancet. 2018;391:541-551.
- Mitri J, Hamdy O. Diabetes medications and body weight. Expert Opin Drug Saf.2009;8:573-584.
- Brazeau AS, Leroux C, Mircescu H, Rabasa-Lhoret R. Physical activity level and body composition among adults with type 1 diabetes. Diabet Med. 2012;29:e402-408.
- Ley SH, Hamdy O, Mohan V, Hu FB. Prevention and management of type 2 diabetes: dietary components and nutritional strategies. Lancet. 2014;383:1999-2007.
- Emadian A, Andrews RC, England CY, et al. The effect of macronutrients on glycaemic control: a systematic review of dietary randomised controlled trials in overweight and obese adults with type 2 diabetes in which there was no difference in weight loss between treatment groups. Br J Nutr. 2015;114:1656-1666.
- Turner-McGrievy GM, Barnard ND, Cohen J, et al. Changes in nutrient intake and dietary quality among participants with type 2 diabetes following a low-fat vegan diet or a conventional diabetes diet for 22 weeks. J Am Diet Assoc. 2008;108:1636-1645.
- Evert AB, Boucher JL, Cypress M, et al. Nutrition therapy recommendations for the management of adults with diabetes. Diabetes Care. 2014;37(suppl 1):S120-S143.
- Carter P, Achana F, Troughton J, et al. A Mediterranean diet improves HbA1c but not fasting blood glucose compared to alternative dietary strategies: a network meta-analysis. J HumNutr Diet.2014;27:280-297.
- Brand-Miller J, McMillan-Price J, Steinbeck K, Caterson I. Dietary glycemic index: health implications. J Am Coll Nutr. 2009;28(suppl):446s-449s.
- Otles S, Ozgoz S. Health effects of dietary fiber. Acta Sci Pol TechnolAliment. 2014;13:191-202.
- Rose DJ. Impact of whole grains on the gut microbiota: the next frontier for oats? Br J Nutr. 2014;112(suppl 2):S44-S49.
- He M, van Dam RM, Rimm E, et al. While-grain, cereal fiber, bran, and germ intake and the risks of all-cause and cardiovascular disease-specific mortality among women with type 2 diabetes mellitus. Circulation. 2010;121:2162-2168.
- Burger KNJ, Beulens JWJ, van der Schouw YT, et al. Dietary fiber, carbohydrate quality and quantity, and mortality risk of individuals with diabetes mellitus. PLoS One. 2012;7:e43127.
- West CE, Renz H, Jenmalm MC, et al. The gut microbiota and inflammatory noncommunicable diseases: associations and potentials for gut microbiota therapies. JAllergy Clin Immunol. 2015;135:3-13; quiz 14.
- Blaut M. Gut microbiota and energy balance: role in obesity. Proc Nutr Soc. 2015;74:227-234.
- Woodman RJ, Chew GT, Watts GF. Mechanisms, significance and treatment of vascular dysfunction in type 2 diabetes mellitus: focus on lipid-regulating therapy. Drugs. 2005;65:31-74.
- Siri-Tarino PW, Sun Q, Hu FB, Krauss RM. Saturated fat, carbohydrate, and cardiovascular disease. Am J Clin Nutr. 2010;91:502-509.
- Gayet-Boyer C, Tenenhaus-Aziza F, Prunet C, et al. Is there a linear relationship between the dose of ruminant trans-fatty acids and cardiovascular risk markers in healthy subjects: results from a systematic review and meta-regression of randomised clinical trials. Br J Nutr. 2014;112:1914-1922.
- Evert AB, Dennison M, Gardner CD, et al. Nutrition therapy for adults with diabetes or prediabetes: a consensus report. Diabetes Care. 2019 Apr 18 [Epub ahead of print].
- Kay CD, Kris-Etherton PM, West SG. Effects of antioxidant-rich foods on vascular reactivity: review of the clinical evidence. Curr Atheroscler Rep. 2006;8:510-522.
- Micha R, Michas G, Lajous M, Mozaffarian D. Processing of meats and cardiovascular risk: time to focus on preservatives. BMC Med. 2013;11:136.
- Ericson U, Sonestedt E, Gullberg B, et al. High intakes of protein and processed meat associate with increased incidence of type 2 diabetes. Br J Nutr. 2013;109:1143-1153.
- Bjermo H, Iggman D, Kullberg J, et al. Effects of n-6 PUFAs compared with SFAs on liver fat, lipoproteins, and inflammation in abdominal obesity: a randomized controlled trial. Am JClin Nutr. 2012;95:1003-1012.
- Alhazmi A, Stojanovski E, McEvoy M, Garg ML. Macronutrient intakes and development of type 2 diabetes: a systematic review and meta-analysis of cohort studies. J Am Coll Nutr. 2012;31:243-258.
- Benatar JR, Sidhu K, Stewart RA. Effects of high and low fat dairy food on cardio-metabolic risk factors: a meta-analysis of randomized studies. PLoS One. 2013;8:e76480.
- Sabate J. Nut consumption and body weight. Am J Clin Nutr. 2003;78(suppl 3):647s-650s.
- Hamdy O, Horton ES. Protein content in diabetes nutrition plan. Curr Diab Rep. 2011;11:111-119.
- American Diabetes Association. 11. Microvascular complications and foot care: Standards of Medical Care in Diabetes – 2019. Diabetes Care. 2019;42(Suppl. 1):S124-S138.
- Brazeau AS, Mircescu H, Desjardins K, et al. Carbohydrate counting accuracy and blood glucose variability in adults with type 1 diabetes. Diabetes Res Clin Pract. 2013;99:19-23.
- Bell KJ, Gray R, Munns D, et al. Estimating insulin demand for protein-containing foods using the food insulin index. Eur J Clin Nutr. 2014;68:1055-1059.
- Wolpert HA, Atakov-Castillo A, Smith SA, Steil GM. Dietary fat acutely increases glucose concentrations and insulin requirements in patients with type 1 diabetes: implications for carbohydrate-based bolus dose calculation and intensive diabetes management. DiabetesCare. 2013;36:810-816.
- Wolever TM, Mullan YM. Sugars and fat have different effects on postprandial glucose responses in normal and type 1 diabetic subjects. Nutr Metab Cardiovasc Dis. 2011;21:719-725.
- Bao J, Atkinson F, Petocz P, et al. Prediction of postprandial glycemia and insulinemia in lean, young, healthy adults: glycemic load compared with carbohydrate content alone. Am JClin Nutr. 2011;93:984-996.
- Peters AL, Davidson MB. Protein and fat effects on glucose responses and insulin requirements in subjects with insulin-dependent diabetes mellitus. Am J Clin Nutr. 1993;58:555-560.
- Bell KJ, Smart CE, Steil GM, et al. Impact of fat, protein, and glycemic index on postprandial glucose control in type 1 diabetes: implications for intensive diabetes management in the continuous glucose monitoring era. Diabetes Care. 2015;38:1008-1015.
- Brand-Miller JC. Postprandial glycemia, glycemic index, and the prevention of type 2 diabetes. Am J Clin Nutr. 2004;80:243-244.
- Bao J, de Jong V, Atkinson F, et al. Food insulin index: physiologic basis for predicting insulin demand evoked by composite meals. Am J Clin Nutr. 2009;90:986-992.
- Franz MJ, MacLeod J, Evert A, et al. Academy of Nutrition and Dietetics Nutrition practice guideline for type 1 and type 2 diabetes in adults: systematic review of evidence for medical nutrition therapy effectiveness and recommendations for integration into the nutrition care process. J Acad Nutr Diet. 2017;117:1659-1679.
- Vega-Lopez S, Venn BJ, Slavin JL. Relevance of the glycemic index and glycemic load for body weight, diabetes, and cardiovascular disease. Nutrients. 2018;10:E1361.
- Chung M, Ma J, Patel K, et al. Fructose, high-fructose corn syrup, sucrose, and nonalcoholic fatty liver disease or indexes of liver health: a systematic review and meta-analysis. Am JClin Nutr. 2014;100:833-849.
- American Diabetes Association. 9. Pharmacologic approaches to glycemic treatment: Standards of Medical Care in Diabetes - 2019. Diabetes Care. 2019;42(Suppl. 1):S90-S102.
- Ding M, Bhupathiraju SN, Chen M, et al. Caffeinated and decaffeinated coffee consumption and risk of type 2 diabetes: a systematic review and a dose-response meta-analysis. DiabetesCare. 2014;37:569-586.
- Jiang X, Zhang D, Jiang W. Coffee and caffeine intake and incidence of type 2 diabetes mellitus: a meta-analysis of prospective studies. Eur J Nutr. 2014;53:25-38.
- Lee S, Hudson R, Kilpatrick K, et al. Caffeine ingestion is associated with reductions in glucose uptake independent of obesity and type 2 diabetes before and after exercise training. Diabetes Care. 2005;28:566-572.
- Lane JD, Feinglos MN, Surwit RS. Caffeine increases ambulatory glucose and postprandial responses in coffee drinkers with type 2 diabetes. Diabetes Care. 2008;31:221-222.
- Robinson LE, Savani S, Battram DS, et al. Caffeine ingestion before an oral glucose tolerance test impairs blood glucose management in men with type 2 diabetes. J Nutr. 2004;134:2528-2533.
- S. Food & Drug Administration. Changes to the nutrition facts label. Available at https://www.fda.gov/Food/GuidanceRegulation/GuidanceDocumentsRegulatoryInformation/LabelingNutrition/ucm385663.htm Accessed April 22, 2019.
Back to Top