
Expired activity
Please go to the PowerPak
homepage and select a course.
Module 3. Collection and Evaluation of Patient-specific Information
INTRODUCTION
Collecting patient-specific information for MTM involves:
- obtaining information from the patient's medical or pharmacy records;
- obtaining information directly from the patient; and
- communicating relevant information to other providers
An overearching goal of MTM is to connect these sources, so the patient understands what has been prescribed, and the prescriber recognizes how the patient is using medical therapies. Based on the information collected, collaborating providers can determine which components of the overall regimen are in the person's best interest.
Obtaining patient-specific information is not necessarily straightforward. Medical history is not always readily available to the pharmacist. And, medication fill/refill records from the pharmacy may be missing from the patient's electronic medical record (EMR). The pharmacist conducting MTM is likely to identify conflicting information between the physician's records and what the patient claims to be taking. Therefore, obtaining information directly from the patient—in a way that elicits open communication and promotes a positive approach to self-care—is a skill that the pharmacist must develop during MTM.
GATHERING INFORMATION IN ADVANCE
Ideally, the pharmacist should begin MTM with access to information about the patient's medical history and medication use. How much data can be gathered in advance often depends upon the practice setting: in hospitals, long-term care settings, or primary care/outpatient clinics, a paper or EMR can often be examined to begin the process of creating a personal medication list (PML) and MTM action plan. Such settings may be considered "data-rich" environments.1
Pharmacists or staff members can initiate contact with the patient's healthcare provider prior to an MTM session to seek medical records or any missing details. Realistically, pharmacists should not rely on receiving timely and complete medical records from other providers. When patients consent to participate in MTM, they should be provided with Health Insurance Portability and Accountability Act (HIPAA) forms that allow sharing of information between physicians and the pharmacy or MTM provider. When the patient signs the form prior to MTM, the pharmacy must keep a copy. The physician's office may request a copy of the signed HIPAA form in order to release information to the pharmacy. If information is being transferred electronically, it's important for the pharmacist to be familiar with firewalls within the organization (e.g., a pharmacy chain) that can help to safeguard patient privacy.2
Physicians' practices are not required to provide patient information to pharmacists without a HIPAA release form; however, the Centers for Medicare & Medicaid Services (CMS) does advise physicians who accept patients on Medicare Part D that MTM providers may be contacting them for information.3 But, the response to requests from doctors' offices for medical records or other patient data may be delayed. Requests may be met with resistance due to a heavy administrative burden in the medical practice or other factors. Sometimes, the patient or caregiver can help in obtaining medical records. However, some medical offices charge patients a fee for this service. Some EMR systems will allow pharmacists and other caregivers to access patient records in a "read-only" format.
At times, little or no background information can be obtained from outside sources. If so, the pharmacist conducting MTM must rely on details supplied by patients and caregivers. Many pharmacists operate in environments where only limited patient information is available in advance of MTM. Community pharmacies may be examples of "data-poor" environments.1
Table 1 contains a checklist of sources for patient information for use in MTM, to be obtained before the MTM meeting and during the interview portion.
|
Table 1. Source Document Checklist
Before MTM session, if applicable
- Electronic medical record (EMR) from primary care physician or outpatient clinic
- In-house pharmacy records
- Medication utilization documents from Part D sponsor or payer (insurance company)
- Hospital discharge instructions
- Recent laboratory results
- Pharmacy claims history (fill history, cost information)
During MTM interview (to be brought by patient/caregiver)
- Medical records or lab results
- Prescription containers (preferable) or lists of medications taken
- Supplements (in original containers when possible)
- Over-the-counter medications, in original packaging if possible
- Symptom diaries, adherence diaries/records kept by patient
- Syringes, inhalers, other devices used by the patient
|
PREPARING THE PATIENT FOR AN MTM SESSION
When confirming patients' MTM appointments over the phone, it is a good idea to remind them to bring along everything related to medication use (see Table 2). This includes old medications (to evaluate for refill or disposal), non-oral formulations (such as patches, topical preparations, and injectable medications), and recent lab reports. Some people are meticulously organized with their medications; others may bring in a jumbled mix of prescription and over-the-counter containers. However, having the actual items at an in-person MTM session provides a more accurate idea of medication names, doses, and number of doses remaining in the container, as opposed to a list based on the patient's own recollection. For example, the patient may choose to bring older prescriptions that are not documented on the medical record—he or she may be unaware of why this was prescribed or whether it should still be taken. So while it may seem time-consuming to sort through all the products, this process can be done as part of an active dialogue with the patient that is likely to yield much information. Many people are "visual thinkers" or have low health literacy levels. Thus, most patients are more likely to answer the question, "How do you take this medicine?" if you are holding the bottle or a tablet, rather than asking by medication name.
Health literacy differs from other types of literacy. Even a person who is highly educated may be unaware of a generic name of a branded medication, mix up the names of drugs being taken, or have difficulty understanding how to interpret the dosage instructions.
|
Table 2. Key Steps to Prepare in Advance for an MTM Session
- Background research
- Obtain available information from pharmacy, medical, or health plan records
Identify patients' apparent diagnoses and chief complaints
- MTM appointment planning
- Note if person will be coming to appointment alone or with a caregiver/relative
Prepare relevant HIPAA forms (these may be needed prior to obtaining information from providers for MTM)
Clearly advise patient/caregiver on what to bring to appointment, including all prescription and over-the-counter medications, laboratory work, etc.
- Setting the stage
- Determine any special needs regarding communication (e.g., need for a translator) or accessibility (e.g., wheelchair access)
Reserve private space where MTM provider and patient can sit comfortably and talk privately
- Assemble forms and background information
- Obtain pharmacy records ahead of time, to avoid searching during the session
Ensure that any permissions or forms requiring the patient's signature are on hand
Gather templates or forms needed to compile the patient's medication list and action plan
|
TIPS AND TECHNIQUES FOR INTERVIEWING THE PATIENT
Making the most out of the time in a face-to-face (or telephone/video) patient interview is a key goal for an MTM session. Use of appropriate interviewing techniques can help to make patients feel comfortable and more open to sharing detailed, often-personal information. For some people, talking about their medications, health problems, and daily habits may be embarrassing or awkward. The principals of motivational interviewing (expressing a non-judgmental attitude, using open-ended questions, reflective listening, and summarizing statements) will further the goals of MTM. Motivational interviewing techniques are covered in Module 5, Communication Essentials and Module 14, Adherence.
Setting the stage
The session should begin with an introduction. ("Good morning, Mrs. Jones. I'm ________. I'll be talking to you about your medications.") If a family member or friend is present, be sure to ask the patient's permission (and give them options) prior to including the other person in the interview session. ("Are you comfortable having your son present, or would you rather call him when we're finished?"). Having a formal meeting with a pharmacist to speak about medications is often a new experience for patients. It is important to discuss general goals for the visit and/or provide background on the pharmacist. The patient should understand that the pharmacist and physician are working as a team, and that any decisions will be handled collaboratively. It is also helpful to elicit the patient's goals for the visit. The pharmacist can ask: "If there is one thing I can do for you related to your medications, what would it be?" Or, "What are you hoping to get out of our visit today?" The pharmacist conducting the MTM interview can help to increase the person's comfort by:
- appearing relaxed—not rushed or distracted
- maintaining eye contact
- avoiding distractions and interruptions
- silencing the phone (if you use it during the visit to obtain drug information, be sure to explain to the patient what you are doing)
Steps in the interview process
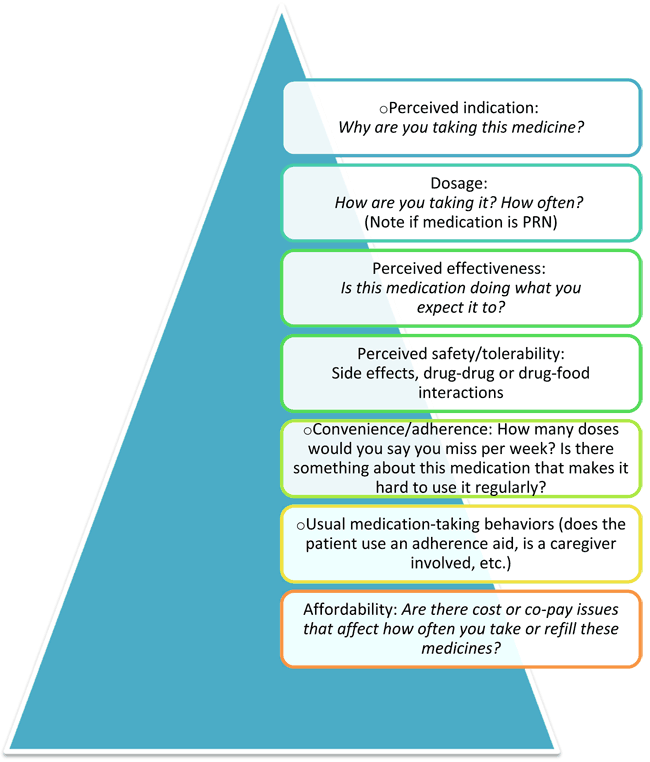
A chief goal in the MTM interview is to establish a rapport with the patient and a sense of trust that will enable the pharmacist to obtain truthful information. A top priority is to establish whether patients recognize the need for their medications. Table 3 and Figure 1 cover the basic recommended steps of the patient interview.
|
Table 3. Steps in the MTM Patient Interview
- Introduce the benefits of MTM: how it's different from usual pharmacy services; why MTM can help the patient to better manage and understand medication use
- Also introduce the pharmacist's background and provide an overview for goals of the visit
- Determine the patient's chief complaint: "What are your main concerns about your medications or healthcare?"
- Gather social history: marital status, living situation, occupation, cooking/eating habits
- Use of alcohol, tobacco, caffeine, illicit drugs
- Past medical history, family medical history
- Allergies and adverse reactions to medications, if any
- Medications tried and failed in the past (and reason why)
- Lab results, blood pressure, weight, pulmonary function testing results, etc.
- Medication-taking behaviors (See Figure 1)
|
| Figure 1. Asking Patients About Medication-Taking Behaviors |
 |
USING SUBJECTIVE AND OBJECTIVE INFORMATION (SOAP)
Some MTM providers follow the "SOAP" system, beginning with Subjective information (based on the patient's opinions and personal understanding of their experience on a medication), followed by Objective information (dosage, administration). Subjective information is anything that cannot be validated with objective evidence. Even laboratory values reported by the patient must be considered subjective unless they can be verified with a lab report or other evidence. SOAP is described in more detail in Figure 2.
Figure 2. Using SOAP Technique to Record Medical Information
Document for each medication (including OTC and supplement) |
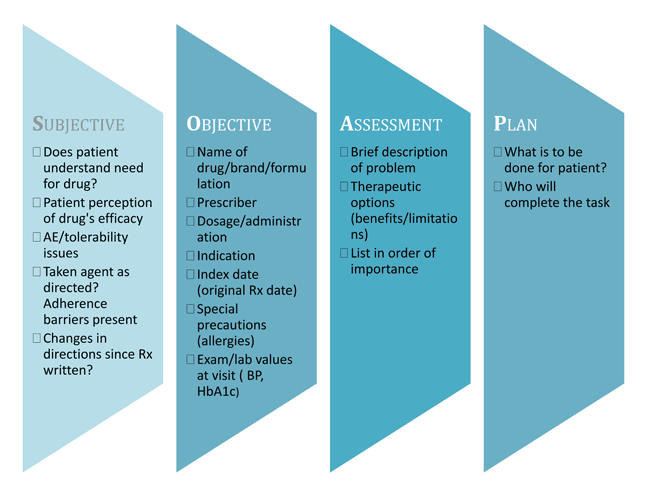 |
Table 4 summarizes the types of information that should be collected during the patient interview.
| Table 4. Summary of Patient and Medication Information |
|
General Patient Demographic and Medical Information
|
· Patient contact and emergency contact information
· Provider contact information (all providers/prescribers)
· All pharmacies being used for prescriptions
· Allergies, including medication allergies
|
|
For Each Medication
|
- Why are you taking this medication?
- Do you believe it is helping you? If so, how?
- What instructions did you receive for its use?
- What dose are you taking now? How often do you miss doses?
- What times of day do you take it? What does "twice daily" or "take 2 tablets daily" mean to you?
- How do you feel when you take it?
- Is there anything about taking this medication that bothers you?
- What warnings or risks worry you? Does this affect the way you take it?
- What about affordability? Do you ever skip doses or avoid refilling the medicine because of the cost?
|
The Personal Medication List: What It Is, What It's Not
The essential take-home document for the patient following an MTM session is the Personal Medication List (PML). Although this document goes by various names, personal medication list is the term used by CMS. According to the Personal Medication List:
"...Is intended to help your patient understand their medications and how they relate to their treatment plans. Your patient can make notes on their Personal Medication List such as when and why they stopped taking a medication."3,4
What It Is:
- A concise record for use by the patient to manage his/her current medication therapies
- Combines medication information with actionable items for the patient
- Able to be shared with other healthcare professionals
- Dated, updated regularly
- Integrated into patient's electronic medical record, if possible
What It is NOT:
- A complete history of all the medications a patient has ever taken
- A heavy discharge summary containing legalese
- A document that contains jargon or acronyms that could be misunderstood by the patient
- A substitute for the Comprehensive Medication Review kept by the pharmacist
The next module discusses the steps for using the information gathered in the MTM interview to develop a strategy that will benefit patients and caregivers, healthcare providers, and the payer/health plan. There are many approaches to doing this, depending on the practice setting.
CONCLUSION
Information-gathering is an essential part of the MTM process. There may seem to be too much information—especially for patients with long medical histories and multiple chronic diseases. It is the role of the pharmacist in MTM to find out whether that information is up-to-date, accurate, and relevant to the patient's current health status and needs, in order to begin the process of fine-tuning the healthcare regimen.
REFERENCES
- Stebbins MR, Cutler TW, Parker PL. Assessment of Therapy and Medication Therapy Management. In: Alldredge BK, Corelli RL, Ernst ME, et al. Koda-Kimble and Youngs Applied Therapeutics: The Clinical Use of Drugs. 10th ed. Baltimore: Wolters Kluwer/Lippincott Williams & Wilkins; 2013.
- HIPAA and Privacy 2013: A survival guide to the law. Pharmacist's Letter. Volume 2013, Course 301. Available at: http://pharmacistsletter.therapeuticresearch.com/ce/cecourse.aspx?pc=13-303.
- Centers for Medicare & Medicaid Services (CMS). A Physician's Guide to Medicare Part D Medication Therapy Management (MTM) Programs. MLN Matters Number SE1229. August 24, 2017. Available at: https://www.cms.gov/Medicare/Prescription-Drug-Coverage/PrescriptionDrugCovContra/Downloads/A-Physician’s-Guide-to-Medicare-Part-D-Medication-Therapy-Management-MTM-Programs-08242017.pdf.
- Centers for Medicare & Medicaid Services (CMS). CY 2019 Medication Therapy Management Program Guidance and Submission Instructions. April 6, 2018. Available at: https://www.cms.gov/Medicare/Prescription-Drug-Coverage/PrescriptionDrugCovContra/Downloads/Memo-Contract-Year-2019-Medication-Therapy-Management-MTM-Program-Submission-v-040618.pdf.
Back Top