
Expired activity
Please go to the PowerPak
homepage and select a course.
Module 5, Part 2. Communication With Physicians and Other Healthcare Providers
How the pharmacist communicates with other healthcare providers about MTM is of equal importance to communication with the patient. Physicians and other providers should be informed throughout the MTM process. To collaborate successfully with other members of the healthcare team, pharmacists need to build mutual relationships based on competency and trust.1 This includes informing prescribers about the initial plans to conduct an MTM interview and providing adequate follow-up after patient consultation. Follow-up communication should involve discussion of recommended medication regimen changes and obtaining permission to implement recommendations.
There are some barriers to effective communication. Most healthcare systems do not yet have seamless electronic medical records (EMR) between different care settings. Therefore, an update in the pharmacist's computer system does not confer an automatic update to the physician's EMR. If a reliable email "firewall" is not in place to securely send electronic communications, many pharmacists must fax requests and medical record updates to the physician's office. Although this consumes staff time (and invites potential errors if a fax is not received or is overlooked), it is sometimes the only available scenario. Telephone communication can be an effective mode of communication but is generally reserved for more urgent questions or follow-up on specific requests.
INTRODUCING PROVIDERS TO MTM
When planning an MTM session, it's a good idea to send introductory communication to the patient's physician/s explaining the overall goals and benefits of MTM. This can be prepared as a form letter and modified for each individual. Pharmacists who are initiating a new MTM service might send a generic letter to a large selection of physicians in the area, encouraging collaboration with these providers for the benefit of their patients. Some of the benefits for the physician are summarized in Table 1. Many physicians who are busy with large patient caseloads may welcome the opportunity for a comprehensive medication review for a selected group of patients. Introductory correspondence can be sent to physicians through various methods, including:
- Phone
- Email or regular mail
- Fax
- Letter sent with patient visit
- EMR staff messaging (within the same group)
| Table 1. Benefits of MTM for Prescriber |
- More efficient patient care (i.e., the pharmacist as the medication expert can identify and resolve medication-related problems effectively)
- More comprehensive patient follow-up
- Improved continuity of care
- Minimization of medication errors, adverse effects, and adverse drug-drug interactions
- Increased adherence to therapy
- Enhanced medication reconciliation
- Reduced duplication of therapy (due to polypharmacy)
|
Patients as advocates for MTM collaboration
Some pharmacists who are providing MTM have found that patients can serve as advocates in obtaining physician cooperation and buy-in to MTM. For example, at his or her next office visit, the patient might hand-deliver a letter about an upcoming MTM session, introducing the pharmacist and notifying the physician that there will be further correspondence.
When planning which healthcare professionals should receive correspondence, the pharmacist should be aware of:
- Multiple providers
- Any recent care transitions (hospital to home, hospital to rehab facility)
- Other providers (e.g., advanced practice nurses, physical therapists, social workers, physician assistants, nutritionists) who may be involved in care
APPROACHES TO PRESCRIBER COMMUNICATION
Pharmacists experienced at conducting MTM have noted that some communication methods are more effective than others when corresponding with physicians. Adequate preparation is essential. Pharmacists should make MTM as patient-specific as possible and complete thorough patient work-ups prior to recommending changes to the prescriber. Offering input without assessing the patient as a whole can negatively impact a physician's reception of MTM services. For example, the pharmacist may make a statement, "Recommend starting the patient on X therapy," without knowing that the patient:
- has previously tried that medication (and may have discontinued due to intolerable adverse effects, inability to obtain appropriate lab monitoring, or lack of efficacy)
- does not want to try that particular therapy
- has a contraindication to the therapy of which the pharmacist may be unaware
- is receiving another agent that is incompatible with therapy
Physicians must make decisions about patient care in an imperfect world; often, the choice of therapy that looks best "by the book" may be one that the physician has already tried and has found to be unsuitable for that patient. If the MTM pharmacist says, "This therapy is recommended," without knowing what has or has not been tried—or other extenuating circumstances relevant to that individual—this feedback is unhelpful to the physician. If the physician consistently receives irrelevant feedback, he or she may be reluctant to continue cooperating with MTM. Some key Do's and Don'ts of provider communication are summarized in Table 2.
| Table 2. Dos and Don'ts for Provider Communication |
- DO emphasize teamwork and collaboration
Stress the benefits to the provider, and any past successes you may have had (without revealing any private patient identifiers). Make recommendations a discussion and be flexible when appropriate.
- DO recognize the patient/provider relationship
Stress that decisions are made on a collaborative basis and are not intended to leave the physician out of the loop.
- DO recognize that you may lack key information
Instead of stating, "Suggest starting the patient on a long-acting insulin," you might say, "If the patient has not already done so, suggest a trial of …"
- DON'T use language that may sound accusatory
Instead saying, "We will eliminate this patient's problems with drug therapy problems" say, "We will attempt to optimize the patient's drug therapy." Instead of saying, "This therapy is not appropriate," say "You may wish to evaluate the continued need for …" or, "This drug may be contributing to/aggravating [adverse effect]."
|
COLLABORATIVE PRACTICE AGREEMENTS AND MTM
Collaborative agreements between physicians and pharmacists can help avoid some of the communication pitfalls described above, because they are less one-sided. These arrangements are intended to provide greater access to and sharing of patient records and ongoing cooperation between healthcare professionals about what therapies are best for the patient.2,3
What is a Collaborative Practice Agreement?
The concept of a collaborative work agreement between physicians and pharmacists is usually known as a collaborative practice agreement (CPA) or collaborative drug therapy management (CDTM).2-5 These formal agreements are arranged in advance between a pharmacist or pharmacy group and a licensed prescriber. They offer the advantage of allowing the pharmacist to operate under protocol to make immediate changes in drug therapy and to provide immediate, on-site delivery of care to patients (such as ordering of pertinent laboratory tests). The progression from typical pharmacist–provider interaction and a CPA is illustrated in Figure 1.6
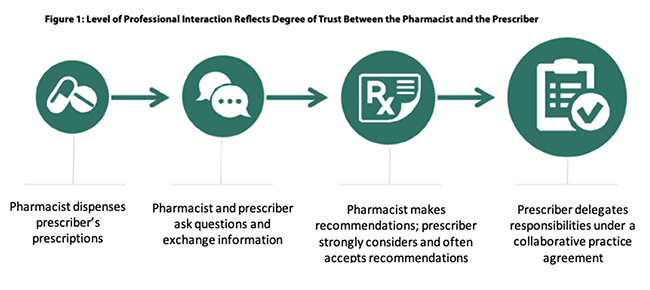 |
| Source: Centers for Disease Control and Prevention (CDC), 2017.6 |
According to Centers for Medicare and Medicaid Services (CMS) guidelines, a "collaborative practice protocol," consists of a written document that identifies drug therapy management actions that a pharmacist is authorized to perform for a patient.7 CMS further states that this document should be developed jointly by the pharmacist and the physician and should include a description of the terms of agreement, including:7
- Identify each physician and pharmacist permitted to participate in a patient's collaborative drug therapy management, including all covering physicians and/or pharmacists;
- Establish the means by which the physician and/or pharmacist will be notified about covering practitioners for collaborative practice purposes;
- Specify functions and responsibilities, including the scope of practice and authority, to be exercised by the pharmacist;
- Indicate any restrictions placed on the use of certain types or classes of drugs or drug therapies;
- Indicate any diagnosis or types of diseases that are specifically included or excluded;
- Include copies of all protocols to be used in the collaborative practice;
- Indicate effective date for the agreement;
- Be signed and dated by physician(s) and pharmacist(s).
The Centers for Disease Control and Prevention (CDC) document, "Advancing Team-Based Care Through Collaborative Practice Agreements: A Resource and Implementation Guide for Adding Pharmacists to the Care Team" contains a sample CPA contract and information about CPA laws in the 50 states (updated as of 2017) https://www.cdc.gov/dhdsp/pubs/docs/CPA-Team-Based-Care.pdf.6
Terms of collaborative practice agreements by state
CPA regulations are constantly evolving at the state level. Currently, 48 states plus the District of Columbia have authorized collaborative agreements between pharmacists and physicians. The two exceptions were Alabama and Delaware. In June 2019 Alabama became the latest state to pass a law allowing CPAs with pharmacists, but this law may not go into effect until October 2019 or later.8
What is permitted under the terms of these agreements is determined on a state-by-state basis.6 The extent of services that can be performed by pharmacists within the CPA also varies from state to state. Some states have stringent restrictions, and others leave more of the decision-making up to the discretion of the provider. For example:
- 38 states currently allow pharmacists to initiate drug therapy under a CPA
- 45 states allow pharmacists to modify existing drug therapy
- In some states, the CPA specifies the medications and/or disease states in which pharmacists can initiate or change therapies. For example, in California a statewide CPA allows all California pharmacists to furnish specific medications/therapies (naloxone, hormonal contraception, travel medicines, immunizations, nicotine replacement therapy).
Once a state has allowed CPA and has define the specific terms, individual organizations can determine (within scope of law) what they will allow pharmacists to do. Services performed by pharmacists under CPAs are not limited to modification of drug therapy and monitoring of laboratory tests. For example, a CPA might include activities such as administering medications to patients who are unable to do so by themselves. In such cases, the physician could order through the CPA that a patient goes to the pharmacy to receive regular medication on schedule.
Some states require minimum credentialing for pharmacists to participate in CPAs. For example, in California CPAs were limited to institution-based pharmacists until the passage of SB 493, which allowed for community pharmacists to enter into CPAs if they had advanced practice pharmacist licensure.9 Other states require specific continuing education or completion of a certificate training program.
The move to increase pharmacists' responsibilities has gained support at multiple levels of government. For example, in 2015 the National Governors Association released a paper supporting full integration of pharmacists into the healthcare system. The paper recommended amendment of existing laws and regulations so pharmacists can practice to the full scope of their training. This was followed by the release of a National Alliance of State Pharmacy Associations (NASPA) Collaborative Practice Workgroup Report which recommended a movement toward national standardization of CPA regulations (Table 3).10
| Table 3. Recommendations on CPAs from the Report of National Alliance of State Pharmacy Associations10 |
|
Recommendations for State Laws/Regulations:
- Any practitioner with prescriptive authority may collaborate with pharmacists using a CPA.
- CPAs may be between a single or multiple pharmacists and a single or multiple prescribers.
- CPAs may apply to a single patient, multiple patients, or patient populations as specified in the agreement.
Elements to be Determined at the Practitioner Level
- CPAs should specify which patient(s) and/or patient population(s) can receive services under the agreement.
- Depending on the complexity of the services being provided under a CPA, it may be appropriate for the pharmacist to have additional credentials or training, beyond what is required for licensure.
- CPAs should specify which pharmacist(s) may provide services under the CPA. A pharmacist's practice setting should not be a barrier to entering into a CPA.
|
What are the benefits of CPAs?
The benefits of CPAs have been studied extensively and described in the literature.11-14 It is important to note, however, that the concept of a CPA is not necessarily synonymous with MTM. A formal agreement of this nature is not required in order for pharmacists to successfully conduct MTM services, but there are clearly benefits to multiple parties in formal collaborative agreements. Collaborative drug therapy management has the potential to benefit multiple parties, as outlined in Figure 2.
Figure 2. Benefits of Collaborative Drug Therapy Management
 |
SUMMARY AND CONCLUSIONS
Pharmacist-physician communication is anticipated to become more formalized as MTM services continue to expand. Pharmacists involved in MTM need to be aware of the types of agreements that can be made with physicians in the specific geographic location and what privileges can be granted through such agreements.
In addition, it behooves pharmacists who are practicing MTM to determine how best to communicate with specific providers without "stepping on toes" or making it appear that they are trying to subvert the physician's authority in patient care. This might mean simply asking the physician, "How would you prefer to communicate," and "What types of suggestions would be valuable to you in the care of this patient?" or, “Do you have a moment to discuss our mutual patient?”
When the pharmacist lacks full background information about a patient, it may be best to state it up front, by saying, "I don't have access to the patient's full medical record, so I don't know if this approach has been tried before. Do you think this recommendation would be appropriate?" This is usually better received than a statement such as "I recommend the patient be placed on drug X." The ultimate goal is to provide patient-centered care. The complexities of the healthcare system require pharmacists to practice effective communication and relationship-building skills in order to be seamlessly integrated into the team.
CPAs allow pharmacists to provide value-added benefits to the healthcare system and to practice to the full extent of their training. CPAs are currently regulated on a state-by-state basis. However, pharmacists should be aware that there is a national movement toward standardizing CPA regulations. Pharmacists should strive to keep up with the rapidly evolving regulatory requirements regarding CPAs.
REFERENCES
- Liu Y, Doucette WR, Farris KB. Examining the development of pharmacist-physician collaboration over 3 months. Res Social Adm Pharm. 2010;6(4):324-333.
- Snyder ME, Zillich AJ, Primack BA, et al. Exploring successful community pharmacist-physician collaborative working relationships using mixed methods. Res Social Adm Pharm. 2010;6(4):307-323.
- Shah B, Chewning B. Conceptualizing and measuring pharmacist-patient communication: a review of published studies. Res Social Adm Pharm. 2006;2(2):153-185.
- Roberts S, Gainsbrugh R. Medication therapy management and collaborative drug therapy management. J Manag Care Pharm. 2010;16(1):67-68.
- McDonough RP, Doucette WR. Dynamics of pharmaceutical care: developing collaborative working relationships between pharmacists and physicians. J Am Pharm Assoc. 2001;41(5).
- Centers for Disease Control and Prevention (CDC). Advancing Team-Based Care Through Collaborative Practice Agreements: A Resource and Implementation Guide for Adding Pharmacists to the Care Team. Atlanta, GA: CDC, U.S. Department of Health and Human Services; 2017. Available at: https://www.cdc.gov/dhdsp/pubs/docs/CPA-Team-Based-Care.pdf
- Centers for Medicare and Medicaid Services. CMS Physician/Non-physician Collaborative Practice Plan Guidelines. Available at: http://www.cms.org/uploads/CollabPracticePlan.pdf
- Alabama Pharmacy Association. HB494: Collaborative Drug Therapy Management: Improving Alabama Patient Outcomes Through Healthcare Collaboration. https://cdn.ymaws.com/aparx.site-ym.com/resource/resmgr/Docs/HB494_CDTM_Talking_Points_Br.pdf
- State of California. CA.gov. SB493 Implementation Regulations. Available at: http://www.pharmacy.ca.gov/laws_regs/.
- National Alliance of State Pharmacy Associations. Pharmacist collaborative practice agreements: Key elements for legislative and regulatory authority. July 2015. Available at: http://naspa.us/wp-content/uploads/2015/07/CPA-Workgroup-Report-FINAL.pdf.
- Cranor CW, Bunting BA, Christensen DB. The Asheville Project: long-term clinical and economic outcomes of a community pharmacy diabetes care program. J Am Pharm Assoc. 2003;43(2):173-184.
- Bunting BA, Smith BH, Sutherland SE. The Asheville Project: clinical and economic outcomes of a community-based long-term medication therapy management program for hypertension and dyslipidemia. J Am Pharm Assoc (2003). 2008;48(1):23-31.
- Fera T, Bluml BM, Ellis WM. Diabetes Ten City Challenge: final economic and clinical results. J Am Pharm Assoc. 2009;49(3):383-391.
- LeBuhn R, Swankin DA. Reforming Scopes of Practice: A White Paper. Washington, DC: Citizen Advocacy Center; 2010. Available at: http://www.ncsbn.org/Reformingscopesofpractice-whitepaper.pdf.
Back Top