
Expired activity
Please go to the PowerPak
homepage and select a course.
INTRODUCTION
Medication reconciliation is the process of determining what medicines a patient has been prescribed and comparing it to what they are taking.1 For many or most patients, it is likely that differences will be found between these two lists. Reconciling the medication list is a standard procedure in most hospitals when a patient is admitted. Pharmacists and technicians often take part in this process.
Medication reconciliation is also a key step in medication therapy management (MTM). MTM starts with the goal of developing a clear, up–to–date medication history. It does not end there. MTM also involves steps to:
- suggest medication changes for purposes related to effectiveness, safety, patient convenience, or economic reasons
- update physicians and other healthcare providers about discrepancies and changes
- educate patients about how to maximize their use of these medications
WHY IS MEDICATION RECONCILIATION IMPORTANT?
Medication reconciliation is often associated with transitions of care. Transitions of care can mean many things, such as admission or discharge from a hospital, switching care providers, or switching health insurance plans.2
After hospital discharge, the medicines a patient was prescribed in the hospital (and is asked to continue taking) might differ quite a bit from those that were prescribed by the patient’s regular physician. Unfortunately, the primary care physician is often not aware of the changes to the patient’s treatment. In addition, the patient may be confused about the changes. For example, a patient who was just discharged from a hospital may wonder, “Which blood pressure medications should I take now? Just the ones prescribed in the hospital? Or, all of them? Now that I’m out of the hospital, should I go back to my usual dose—or stay on this higher one?”3
Medication reconciliation has been formally defined as:
“A process in which the patients’ medication history and changes in drug prescribing information [during transitions of care] are identified using multiple medication information resources."4
In MTM, medication reconciliation one of steps involved in developing the personal medication list (PML). With a current, updated list of medications and background information, the pharmacist can sit down with the patient during MTM to dig deeper. The goal now will be to find out which of these medications are being used as directed, which ones might be changed or eliminated, and how to address any adherence barriers.
PHARMACY TECHNICIANS’ ROLE IN RECONCILIATION FOR MTM
Pharmacy technicians can manage many of the steps involved in medication reconciliation for MTM, regardless of the care setting.5 When technicians are trained effectively, studies have shown that their accuracy in reconciliation is similar to that of pharmacists.6,7 Other studies have shown that technicians who are responsible for medication reconciliation in hospitals can detect more errors than other professionals, such as doctors and nurses, in performing these tasks.3 While nurses and physicians have traditionally collected patient medication histories, their ability to obtain complete and accurate records may be limited by heavy patient caseloads and interruptions related to patient care.
- A Dutch study of patients being prepped for surgery showed that pharmacy technicians were better able to reduce medication–related discrepancies in the record (5% error rate), compared with anesthesiologists (38% error rate).8 (A “discrepancy” was when drug information entered into the chart by the patient’s physician differed from what the patient was actually taking.)
- A 2015 study in a Florida hospital compared the accuracy of medication histories conducted in the emergency department (ED) by pharmacy technicians versus those done by nurses. The histories conducted by the technicians were accurate 88% of the time, versus 57% for nurses (Figure 1).9
| Figure 1. Percent Accuracy of Pharmacy Technicians in Comparison to Nurses9 |
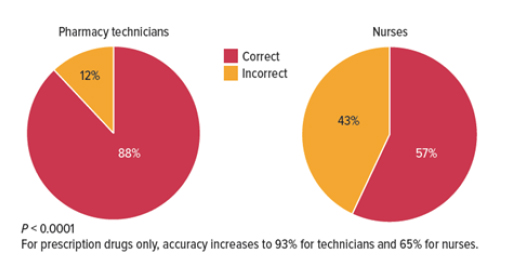 |
| From: Hart C, et al. A program using pharmacy technicians to collect medication histories in the emergency department. P T. 2015;40(1):56-61. |
- A study from a North Carolina hospital evaluated how well a pharmacy team performed medication reconciliation services. Pharmacy technicians obtained patient histories, while pharmacists reviewed the histories and reconciled the results against admission orders. Accuracy of the findings increased from 46% with a multidisciplinary approach (involving physicians and nurses) to 95% when the pharmacy team did the medication reconciliations.1
Why is the pharmacy team—a combination of clinical pharmacists and pharmacy technicians, and pharmacy students or "learners"— well suited to perform reconciliation? Pharmacists and technicians have specialized training in medications, and can focus on the task of obtaining a patient history and fact–finding to follow up the information. By having pharmacy technicians assist with medication reconciliation, pharmacists can focus on overseeing this work and on handling more complex cases.
In the state of California, a law passed in 2019 requires pharmacy staff at hospitals that have more than 100 beds to obtain an accurate medication list for each newly admitted high-risk patient. "Making pharmacy responsible for reconciling these patients’ medication lists removes ambiguity from the process," the legislators stated.10
Many of the research studies on reconciliation by technicians have been based in hospitals. However, these same principles apply to MTM in other settings. Getting technicians involved in the fact–finding and information–gathering process can make the process of MTM more efficient and allow pharmacists to oversee and complete more MTM cases.
“Pharmacy technicians can be employed to devote the majority of their efforts to documenting accurate and comprehensive information. Well–trained pharmacy technicians are proficient in communication techniques and problem–solving abilities, and they possess a fundamental understanding of medication use."9
WHAT KIND OF DISCREPANCIES CAN WE EXPECT DURING RECONCILIATION?
The most common kinds of errors found in the patient’s medical record (or medication record) during medication reconciliation are incorrect or missing doses. This means the record lists a different dose than what the patient is being given, or does not list the dose (Figure 2).9 Other common errors included a missing frequency at which the drug should be taken, and duplicate therapies.
- A “commission” means that the record lists a drug that the patient is not actually taking.
- An “omission” error is related to an action not taken. An example might be a patient who has not filled a prescription. Another example of an omission error would involve failure of the medical record to document a drug that patient is taking.
| Figure 2. Total Errors by Category |
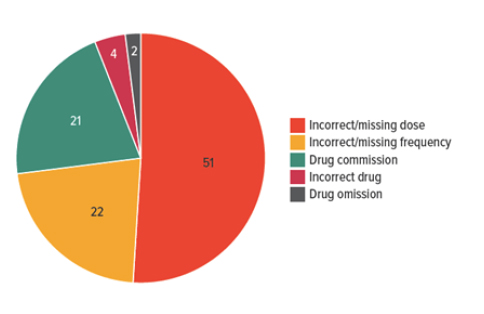 |
| From: Hart C, et al. A program using pharmacy technicians to collect medication histories in the emergency department. P T. 2015;40(1):56-61.9 |
HOW DO WE TRACK DOWN THE INFORMATION NEEDED FOR MTM?
Collecting medication information for MTM involves obtaining information:
1) from the patient’s medical record, including electronic health record (EHR)
2) from pharmacy records, including outside records such as mail order prescriptions
3) directly from the patient and/or caregivers
Pharmacy technicians can contact the patient’s physician before an MTM session to seek medical records or clarify any missing details. Doctors who accept Medicare patients will receive notices from the Centers for Medicare & Medicaid Services (CMS) telling them that they may be contacted by MTM providers (e.g., pharmacists) for information about their patients.11 However, it may not be realistic to expect timely and complete medical records from other providers. This may be due to a heavy administrative burden in the medical practice, or other factors. Sometimes, asking the patient or caregiver to obtain records from a physician can help facilitate the process. (Some medical offices charge patients a fee for this service.) Some EHR systems will allow pharmacists and other caregivers to access patient records in a “read–only” format. At times, there is little or no background information available from outside sources. If so, the process must rely mainly on details supplied by the patient and/or caregiver.
The term "interoperability" in healthcare means the ability for organizations to exchange, interpret and use data cohesively. Most experts evaluating this concept argue that greater interoperability is essential going forward—especially now that more healthcare delivery is relying on technology—but "we're not there yet."12,13
Figure 3 lists some sources that a technician can check before an MTM session, if applicable.
Figure 3. Sources to Check Before an MTM Session
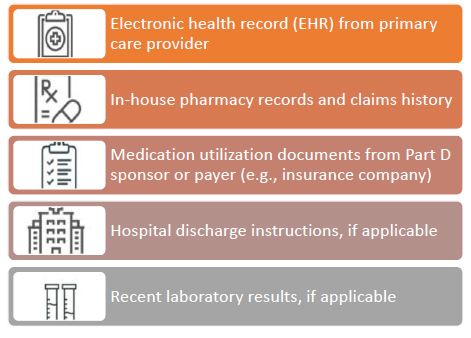
When patients consent to participate in MTM, they should be provided with Health Insurance Portability and Accountability Act (HIPAA) forms that allow sharing of information between physicians and the pharmacy or MTM provider.14 If information is being transferred electronically, it’s important to be familiar with firewalls within the organization (e.g., a pharmacy retail chain) that can help to safeguard patient privacy.
GETTING THE PATIENT’S SIDE OF THE STORY
Pharmacy technicians may have the role of calling patients to remind and prepare them for an MTM meeting. When asked to come in for a meeting, the patient (or caregiver) should be encouraged to bring along all the medications he or she may be taking—or is supposed to be taking—in a brown bag, gym bag, or another container. This should include over–the–counter medications, topical medications, supplements, pill organizer boxes, and administration devices such as syringes. Having the actual items in hand provides a more accurate picture of the medication names, doses, and the number of doses remaining in the container than would a written list or the patient’s recollection (Figure 4). For example, the patient may choose to bring some older prescriptions that are not documented on the physician’s record. He or she may not be aware of why they are being taken, or whether they should still be taken.
Figure 4. What to ask patients to bring to in-person or phone MTM appointments

It may seem time-consuming to pick through all these containers, but this process can be done as part of an active dialogue with the patient that is likely to yield much information. Many people are “visual thinkers” and/or have low health literacy levels. When asked “How do you take this medicine?” patients are more likely to be able to answer when the pharmacist is holding the bottle or individual tablet, rather than being asked by medication name.
HEALTH LITERACY
Health literacy is very different from other types of literacy. It’s important to keep in mind that anyone—even someone who is highly educated—may be unaware of the generic name of a branded medication, or may mix up the names of one or more of the drugs being taken.
Barriers to getting an accurate medication history may include:
- patient confusion or impaired memory
- clinical status (i.e., fatigue, decreased alertness, distraction due to pain)
- outdated information in medical or hospital records
- polypharmacy
- limited access to patient records
- time constraints
- language or cultural differences
PROTOCOLS FOR RECONCILIATION
Using protocols and checklists is a good way to make sure that all the bases are covered when doing a medication reconciliation or medication history. An example of a form used in reconciliation by pharmacists and pharmacy technicians in MTM is shown in Figure 5. In some cases, technicians may be involved in interviewing patients as part of MTM. Information to be obtained from the patient during MTM is summarized below.
| Figure 5. Sample Medication Reconciliation Form |
|
Patient Name, Other identifiers (DOB, Patient #) ___________________________________
Contact information for patient: _______________________________
Emergency contact: ________________________________________
Primary care provider: ______________________________________
Other healthcare providers ___________________________________
Date _______ Ht _______
Wt ____lbs ____oz [Indicate Actual or Stated]
Allergies
|
Meds/Foods/Dyes/Latex/Other
|
Reaction
|
| |
|
| |
|
| |
|
Information obtained from: (Check all that apply)
Patient _______________________________
Family/caregiver _________________________
Prior records [specify] _________________________
Medication _______________________________
Other _______________________________
Initial Medication List
| Medication |
Prescriber/Date prescribed |
Dose/Frequency |
Comments (problems, AEs) |
Source of information* |
| |
|
|
|
|
| |
|
|
|
|
| |
|
|
|
|
| |
|
|
|
|
*(e.g, electronic medical record, pharmacy records, patient recall, patient 'brown bag'
Post MTM Medication List
| Medication |
Prescriber/Date prescribed |
Dose/Frequency |
Comments (problems, AEs) |
Change recommended by pharmacist in MTM? |
| |
|
|
|
|
| |
|
|
|
|
| |
|
|
|
|
| |
|
|
|
|
Follow-up steps required:
_______________________________________________________________
_______________________________________________________________
_______________________________________________________________
[Example: Physician follow-up, blood or other tests needed, follow-up with patient on [date]
|
General patient demographic and medical information:
□ Patient contact and emergency contact information
□ Provider contact information (all providers/prescribers)
□ All pharmacies that have been used to fill prescriptions
□ Allergies (including medication allergies, latex allergies, contrast agents)
During patient interviews, ask about each medication:
□ Why are you taking this medication? What purpose does the medication have?
□ What dose are you taking now? How often do you miss these doses?
□ How are you taking it? (How many times per day, with/without food)
□ Are there any effects of this medication that bother you?
□ Do you ever skip doses, or avoid refilling the medicine because of the cost?
THE PERSONAL MEDICAL RECORD: WHAT IT IS, WHAT IT’S NOT
The essential take–home document for the patient following an MTM session is the Personal Medication List (PML).11,15. The PML is a new list of what medications the patient should be taking, now that the treatment plan has been optimized through MTM.
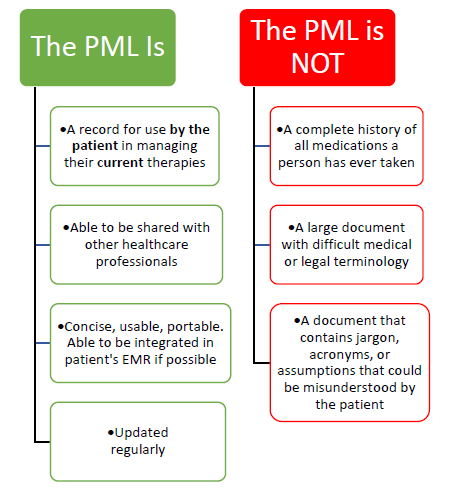
CONCLUSION
Collecting medication information and reconciling the information—by correcting it or filling in the blanks—is part of the MTM process. During MTM, the pharmacist and the pharmacy technician find out which of that information is up–to–date, accurate, and relevant to the patient’s current health status and needs, in order to begin the process of fine–tuning the patient’s treatment plan.
Freeing up pharmacists' time has been of particular relevance during the COVID-19 pandemic. Many community clinics closed in the early months, while pharmacies remained open, providing the only access to medical services for many people.16 As stated in an editorial in the Journal of the American College of Clinical Pharmacy:16
"Pharmacists are a trusted and accessible resource for the public during this public health emergency, especially community pharmacists."
REFERENCES
- Smith SB, Mango MD. Pharmacy-based medication reconciliation program utilizing pharmacists and technicians: a process improvement initiative. Hosp Pharm. 2013;48(2):112-119.
- The Joint Commission. Transitions of Care: The need for a more effective approach to continuing patient care. Available at: https://www.jointcommission.org/-/media/deprecated-unorganized/imported-assets/tjc/system-folders/topics-library/hot_topics_transitions_of_carepdf.pdf?db=web&hash=CEFB254D5EC36E4FFE30ABB20A5550E0.
- Wong JD, Bajcar JM, Wong GG, et al. Medication reconciliation at hospital discharge: evaluating discrepancies. Ann Pharmacother. 2008;42(10):1373-1379.
- Buck TC, Gronkjaer LS, Duckert ML, et al. Medication reconciliation and prescribing reviews by pharmacy technicians in a geriatric ward. J Res Pharm Pract. 2013;2(4):145-150.
- Hart C. Using pharmacy technicians to improve the accuracy of medication histories collected in the ED. Pharmacy Practice Model Initiative (PPMI). American Society of Health-System Pharmacists. Available at: http://www.ashpmedia.org/pai/docs/casestudy_Hart.pdf.
- Buckley MS, Harinstein LM, Clark KB, et al. Impact of a clinical pharmacy admission medication reconciliation program on medication errors in "high-risk" patients. Ann Pharmacother. 2013;47(12):1599-1610.
- Johnston R, Saulnier L, Gould O. Best possible medication history in the emergency department: comparing pharmacy technicians and pharmacists. Can J Hosp Pharm. 2010;63(5):359-365.
- van den Bemt PM, van den Broek S, van Nunen AK, et al. Medication reconciliation performed by pharmacy technicians at the time of preoperative screening. Ann Pharmacother. 2009;43(5):868-874.
- Hart C, Price C, Graziose G, et al. A program using pharmacy technicians to collect medication histories in the emergency department. P t. 2015;40(1):56-61.
- Thompson CA. California Pharmacists to Ensure Accuracy of High-Risk Patients' Admission Medication Lists. American Society of Hospital Pharmacists (ASHP). Nov 2018. Available at: https://www.ashp.org/news/2018/11/21/california-pharmacists-to-ensure-accuracy-of-high-risk-patients-admission-medication-lists?loginreturnUrl=SSOCheckOnly.
- Centers for Medicare & Medicaid Services (CMS). A Physician's Guide to Medicare Part D Medication Therapy Management (MTM) Programs. MLN Matters Number SE1229.
- Fennelly O, Cunningham C, Grogan L, et al. Successfully implementing a national electronic health record: a rapid umbrella review. Int J Med Inform. 2020;144:104281.
- Kataria S, Ravindran V. Electronic health records: a critical appraisal of strengths and limitations. J R Coll Physicians Edinb. 2020;50(3):262-268.
- Tariq RA, Hackert PB. Patient Confidentiality. StatPearls. Treasure Island (FL): StatPearls Publishing; 2020.
- Centers for Medicare & Medicaid Services (CMS). Medication Therapy Management Program Guidance and Submission Instructions. May 22, 2020. Available at: https://www.cms.gov/files/document/memo-contract-year-2021-medication-therapy-management-mtm-program-submission-v-052220.pdf.
- Gross AE, MacDougall C. Role of the clinical pharmacist during the COVID-19 pandemic. J Am Coll Clin Pharmacy. Mar 30, 2020. Available at: https://accpjournals.onlinelibrary.wiley.com/doi/full/10.1002/jac5.1231.